Primary goal of attending an international conference is to present a paper to the experts and influencers. It gives you a platform to exchange your interest-related thoughts, paving the way for possible future collaborations.

Use this platform to build connections with an elite group of wise men and women to enhance your intellect. Young entrepreneurs, this is a great platform to connect with your peers.

Knowledge is Power. Knowledge teaches skills. Skills define excellence. Use this platform to become cognizant of your interest area to achieve excellence in your domain.

Attending a conference give you opportunity to get your abstract or paper published in conference proceedings

Meet and greet a myriad of industry professionals and academia experts with common interest. Every meal will be an opportunity to meet and interact with fellow researchers, attendees and experts.

Expand your professional competency and learn useful tips and tricks of your industry in our skill-building workshops.

Explore insights on recent advancements, new equipment, new techniques, and unpublished data, learn from thought-leaders and get to network with a great line up of speakers.

Our exhibits floor offers the attendees with a dynamic display of the latest products with cutting-edge technology.

Investing in you is the best investment. Peers Alley conferences give the patrons with a feeling of the serendipity of real learning, skill development in strategic workshops, networking and start-up opportunities, thus, is value for money.

Attending the conference gives you much needed break from your regular duties. It also allows you to explore new cities, culture and meet new people. You will feel energized and rejuvenated to return to the university and continue with the job after attending the conference.
Conferences are vital forum for academic researchers and business leaders. "It involves multiple presentations, interactive breakout sessions, hands-on product demonstrations and unrivalled networking opportunities".
We have invited some of the world's most sought-after keynote speakers, experts, brand ambassadors, and industry leaders to share their thoughts and ideas with our conference guests.
Register Now
Advance Cardiology Proceedings 
Dear Colleagues and Friends,
We are pleased to extend a warm welcome to all professionals and academics from all over the world to Berlin, Germany for the 4th Global Conclave on Advanced
Cardiology and Cardiovascular Innovations, which will be held from June 26-27, 2025.
The cardiology conference brings together experts in the field to give you the best education possible. The scientific program has been created to offer a summary of the most recent advancements in the diagnosis and treatment of cardiovascular (CV) disease, with a focus on arrhythmias, structural heart disease, coronary artery disease, heart failure, valvular heart disease, preventative cardiology, and innovations in cardiology. This conference represents a steadfast investment in education as well as a solid portfolio of translational and clinical research.
Many distinguished cardiologists and scientists will participate in this congress. Papers will be presented in plenary sessions, distinguished speaker sessions, workshops, symposia, and posters includes excellent scientific material. These studies, which come from laboratories in 50+ countries, to ensure that the meeting will be a major scientific event. The scientific program will also feature a number of case studies with faculty members that will highlight both common and complicated coronary, peripheral, and structural problems.
Adv.Cardiology 2025 will also let industries to demonstrate their latest products, devices, and medical instruments to cardiologists. I invite you all to attend and make this meeting a grand success.
Sincerely yours,
Adv. Cardiology 2025
Organizing Committee
Peers Alley Media, 1126 59 Ave East, V5X 1Y9, Vancouver BC, Canada

NYU Grossman Long Island School of Medicine, USA

Massachusetts General Hospital, USA

Saint Louis University, USA

University of Minnesota, USA
Cardiology: A Deep Dive into the Heart's Specialists
Cardiology, a branch of internal medicine, is a medical discipline focused on the diagnosis, treatment, and prevention of diseases and conditions of the heart and vascular system. At the center of this specialty stands the cardiologist, a medical doctor specifically trained to address the complex needs of the heart.
Role of a Cardiologist:
A cardiologist is tasked with managing various heart-related conditions, which include:
Coronary Artery Disease (CAD): A condition where the arteries supplying the heart become narrowed or blocked.
Arrhythmias: Irregularities in the heart's rhythm, which might manifest as tachycardia (fast heartbeat) or bradycardia (slow heartbeat).
Congenital Heart Defects: Malformations of the heart present at birth.
Heart Failure: A situation where the heart cannot pump blood effectively to meet the body's demands.
Valvular Heart Diseases: Issues with one or more of the heart's four valves, which might include stenosis or insufficiency.
There are several sub-specialties within cardiology, including:
Interventional Cardiology: Focuses on catheter-based treatments for heart diseases, such as angioplasty and stent placement.
Electrophysiology: Concentrates on the heart's electrical system and treats irregular heart rhythms.
Cardiac Imaging: Uses sophisticated imaging methods, like echocardiography or cardiac MRI, to diagnose heart conditions.
Heart Failure and Transplant Cardiology: Focuses on patients with advanced heart failure and those undergoing or who have undergone heart transplants.
Cardiologist vs. Cardiac Surgeon
While both professionals focus on heart health, they have distinct roles:
Cardiologist: Primarily diagnoses and treats heart diseases using non-surgical methods. However, interventional cardiologists can perform certain procedures like angioplasties.
Cardiac Surgeon: A specialist who performs heart surgeries, including coronary bypass grafting, heart transplants, and surgeries to repair or replace heart valves.
Subtopics
General clinical cardiologists | Electro physiologist | Nuclear cardiologists | MR/CT cardiologists | Pediatric cardiologists | Heart failure & transplant cardiologist | Preventive cardiologists | Vascular medicine specialists | Cardiovascular investigators | Cardiac anesthesiologists
Market Statistics:
The cardiology Surgical & Interventional Cardiology Devices Market was valued at $ 17.95 billion in 2019 and is expected to grow at a CAGR of 7.65% between 2020 and 2025.
Tags
Cardiology Conferences 2024
Arrhythmia Conferences
Stroke Conferences
Cardiology Conferences 2024 Canada
Cardiology Conferences 2024
Peers Alley Media Conferences
Hypertension Conferences
Clinical Cardiology Conferences
Heart Congress Japan
Cardiology Conferences 2024 Asia
Vascular Biology Conferences
Pediatric Cardiology Conferences
Cardiac Imaging Conferences
Cardiology Conferences 2024 Europe
Clinical Cardiology: The Heart of Patient Care
Clinical cardiology is a crucial facet of the broader cardiology discipline, emphasizing patient care, diagnosis, management, and nonsurgical treatments of cardiovascular diseases. While the realm of cardiology extends to research, diagnostics, and surgical interventions, clinical cardiology zeroes in on direct patient management and care.
Scope of Clinical Cardiology:
Diagnosis: Clinical cardiologists use a battery of tests to diagnose heart conditions. Common tests include electrocardiograms (ECG or EKG), Holter monitoring, stress tests, echocardiograms, and cardiac catheterization.
Management: Once a diagnosis is established, clinical cardiologists outline a management plan tailored to the patient's condition. This could involve medications, lifestyle recommendations, or coordination with other specialists for procedures.
Prevention: A cornerstone of clinical cardiology is preventing heart diseases. This encompasses educating patients about risk factors, offering strategies to manage these risks, and early intervention if risk factors are identified.
Continual Care: For many cardiovascular conditions, ongoing management is necessary. Clinical cardiologists oversee the long-term care of patients, adjusting treatment plans as necessary and monitoring progression or improvement.
Collaboration: Clinical cardiologists often work in tandem with other specialists, especially when a patient needs interventional or surgical treatments. This multidisciplinary approach ensures comprehensive care.
Technological Advancements in Clinical Cardiology:
The field has witnessed rapid technological advancements, transforming patient care:
Wearable Tech: Devices like smartwatches now have the capability to monitor heart rhythms, offering a non-invasive way to keep an eye on heart health and even detect atrial fibrillation.
Telemedicine: Especially useful for routine check-ups and patients living in remote areas, telemedicine facilitates consultations through digital platforms.
Advanced Imaging: Techniques like 3D echocardiography, cardiac MRI, and CT angiography offer detailed insights into heart structures and function.
Genetics and Personalized Medicine: Understanding a patient's genetic predisposition can guide treatments and management strategies.
Challenges in Clinical Cardiology
With the advancements, there come challenges:
Keeping Pace with Technology: The rapid pace of technological evolution requires cardiologists to continually update their knowledge and skills.
Multidisciplinary Integration: Collaborating seamlessly with other specialties, especially in large healthcare systems, can be challenging.
Patient Compliance: Ensuring patients adhere to medication and lifestyle recommendations remains a perennial challenge.
Subtopics
Cardiovascular medicine | Preventive medicine | Sleep medicine | Percutaneous Coronary Intervention (PCI) | Modern practices in cardiovascular therapy
Market Statistics:
The global cardiovascular market is approximately $259.1 billion, of which $187 billion is for therapy and $72.1 billion is for devices. The cardiovascular market in the United States is approximately $81.35 billion, with therapy accounting for $50.49 billion and equipment accounting for $30.86 billion.
Tags
Cardiology Conferences 2024 Canada
Heart Diseases Conferences
Cardiology Conferences 2024 Asia
Cardiac Nursing Conferences
Heart Congress Japan
Arrhythmia Conferences
Peers Alley Media Conferences
Cardiology Conferences 2024 Australia
Cardiology Conferences USA
Hypertension Conferences
Cardiology Conferences 2024
Cardiology Conferences 2024 Europe
Vascular Biology Conferences
Stroke Conferences
Heart Diseases: An Overview of the Silent Epidemic
Heart diseases, often referred to as cardiovascular diseases (CVD), encompass a range of conditions affecting the structure and function of the heart. They remain the leading cause of death globally, underscoring the importance of awareness, prevention, and treatment.
Types of Heart Diseases
Coronary Artery Disease (CAD): This is the most common type of heart disease. CAD occurs when the coronary arteries, which supply the heart muscle with oxygen-rich blood, become narrowed or blocked due to a build-up of fatty deposits called plaques. This can lead to angina (chest pain) or a heart attack.
Heart Failure: Contrary to its name, heart failure doesn't mean the heart has completely stopped working. It means the heart isn't pumping blood as efficiently as it should. Causes include CAD, high blood pressure, and diabetes.
Arrhythmias: These are abnormal heart rhythms. The heart can beat too fast, too slow, or irregularly. Examples include atrial fibrillation, tachycardia, and bradycardia.
Valvular Heart Diseases: Conditions affecting the four valves of the heart. Issues can include stenosis (narrowing), regurgitation (backward flow), or prolapse (improper closing).
Congenital Heart Diseases: These are malformations of the heart present at birth. Examples include septal defects and pulmonary stenosis.
Cardiomyopathies: A group of diseases that affect the heart muscle, causing it to enlarge, stiffen, or become thickened. It can lead to arrhythmias or heart failure.
Pericardial Diseases: Conditions affecting the pericardium, the thin sac-like structure surrounding the heart. Pericarditis, an inflammation of this lining, is a common condition in this category.
Risk Factors
Several factors can increase one's risk of developing heart diseases:
Unmodifiable Risks: Age, gender, and genetics/family history.
Modifiable Risks: High blood pressure, high cholesterol, obesity, sedentary lifestyle, tobacco use, excessive alcohol consumption, and an unhealthy diet.
Medical Conditions: Diabetes, chronic kidney disease, and some autoimmune conditions can heighten the risk.
Prevention and Treatment
Lifestyle Choices: Adopting a healthy diet, engaging in regular exercise, avoiding tobacco, limiting alcohol, and managing stress can significantly reduce the risk of heart diseases.
Medications: Depending on the specific heart condition, various medications can be prescribed, such as antihypertensives, statins, or anticoagulants.
Interventions: Procedures like angioplasty, stent placement, and bypass surgery can be employed to treat CAD. Arrhythmias might be managed with pacemakers or defibrillators.
Surgery: In severe cases, especially with valvular heart diseases or congenital defects, surgery might be necessary.
Subtopics
Coronary artery diseases | Atrial fibrillation | Angina | Heart attack | Ischemia Heart Disease | Cerebrovascular disease | Inflammatory Heart Disease
Market Statistics:
From $12.2 billion in 2014 to $22.5 billion in 2021, the market for technologies and goods used to treat coronary heart disease is expected to expand.
Tags
Cardiology Conferences 2024
Heart Conferences
Cardiac Surgery Conferences
Cardiology Conferences 2024 Asia
Cardiology Conferences 2024
Peers Alley Media Conferences
Cardiology Conferences 2024 Australia
Cardiology Conferences USA
Cardiologist Conferences
Cardiac Imaging Conferences
Heart Congress Japan
Stroke Conferences
Heart Diseases Conferences
Arrhythmia Conferences
Hypertension Conferences
Hypertension: The Silent and Pervasive Threat
Hypertension, commonly referred to as high blood pressure, is a condition where the force of the blood against the walls of the arteries is consistently too high. Often labeled as the "silent killer" because of its lack of distinct symptoms, hypertension is a primary risk factor for a multitude of cardiovascular diseases.
Understanding Blood Pressure Readings
Blood pressure is measured in millimeters of mercury (mmHg) and is provided as two readings:
Systolic Pressure: Represents the force exerted on artery walls when the heart contracts or beats. It's the higher of the two numbers.
Diastolic Pressure: Represents the force exerted on artery walls when the heart is at rest between beats. It's the lower number.
A normal blood pressure reading is typically around 120/80 mmHg. Hypertension is usually diagnosed when a person's blood pressure reading consistently exceeds 140/90 mmHg, although the exact threshold can vary based on different guidelines.
Types of Hypertension
Primary (Essential) Hypertension: This is the most common type, with no identifiable cause. It tends to develop gradually over time due to a combination of genetic factors and lifestyle choices.
Secondary Hypertension: Caused by an underlying health condition or medication. Examples include kidney disease, adrenal gland tumors, or medications like birth control pills.
Risk Factors
Several factors can increase the risk of developing hypertension:
Age: Hypertension is more common in individuals as they age.
Race: Certain ethnicities, like African Americans, are at a higher risk.
Family History: Genetics play a role in hypertension development.
Obesity: Excess weight can increase the heart's workload, leading to high blood pressure.
Dietary Choices: High salt intake, excessive alcohol, and lack of potassium can contribute.
Physical Inactivity: Sedentary lifestyles increase the risk.
Tobacco Use: Chemicals in tobacco can damage blood vessel walls.
Complications
If not managed, hypertension can lead to severe complications:
Heart Diseases: Such as heart attacks or heart failure.
Stroke: High blood pressure can cause blood vessels in the brain to rupture or leak.
Kidney Damage: Can lead to kidney failure or kidney scarring.
Vision Loss: Due to damage to the blood vessels in the eyes.
Sexual Dysfunction: Especially common in men.
Management and Treatment:
Lifestyle Changes: Dietary improvements (like the DASH diet), reducing salt intake, increasing physical activity, weight management, limiting alcohol, and stress reduction can all play roles in controlling hypertension.
Medication: There are several classes of anti-hypertensive medications, including diuretics, beta-blockers, ACE inhibitors, calcium channel blockers, and others. The specific medication or combination is tailored to the patient's needs.
Regular Monitoring: Individuals diagnosed with hypertension should routinely monitor their blood pressure to ensure it's within target ranges.
Subtopics
Hypertension | Pulmonary Hypertension | Pediatric Hypertension | Gestational Hypertension | Resistant Hypertension | Sexual dysfunction in Hypertensive patients | Hypertension in diabetes patients | Renal hypertension | Hypertensive heart diseases | Stroke in Hypertensive patients | Obesity in Hypertensive patients | Hypertension Risk Factors, Diagnosis and Treatment | Hypertension Epidemiology | Cardiology | Cardiovascular disease
Market Statistics:
The hypertension market is the largest among the various heart disorders, accounting for $32 billion in prescription drug sales in 2018. The market is predicted to increase at a CAGR of 1.7% from 2018 to 2028.
Tags
Cardiology Conferences 2024
Arrhythmia Conferences
Cardiology Conferences 2024 Europe
Peers Alley Media Conferences
Heart Congress Japan
Cardiology Conferences 2024 Canada
Cardiology Conferences USA
Stroke Conferences
Cardiology Conferences 2024 Australia
Hypertension Conferences
Cardiology Conferences 2024
Clinical Cardiology Conferences
Heart Conferences
Vascular Biology Conferences
Cardiac Nursing Conferences
Electrocardiography: Deciphering the Heart's Electrical Activity
Electrocardiography (ECG or EKG) is a diagnostic procedure that records the electrical activity of the heart over a period of time. It provides essential insights into the heart's rhythm and electrical conduction system, helping to identify a myriad of cardiac abnormalities.
Basics of Electrocardiography
At the heart of electrocardiography is the concept that every heartbeat is triggered by an electrical impulse, usually originating from the heart's natural pacemaker—the sinoatrial (SA) node. This electrical activity can be detected and recorded using electrodes placed on the skin.
The ECG Waveform
An ECG tracing is characterized by different waves and segments, each representing specific phases of the cardiac cycle:
P Wave: Represents atrial depolarization (the electrical stimulation of the atria).
QRS Complex: Represents ventricular depolarization (the electrical stimulation of the ventricles). It's the most noticeable part of the ECG waveform.
T Wave: Represents ventricular repolarization (the return of the ventricles to their resting state).
Intervals and segments in the ECG, such as the PR interval or the ST segment, provide further information about the time it takes for impulses to travel through the heart's conduction system and the relative health of the heart muscle.
Clinical Uses of Electrocardiography
Arrhythmia Detection: ECG can identify irregular heart rhythms, like atrial fibrillation, ventricular tachycardia, or heart blocks.
Myocardial Infarction (Heart Attack) Diagnosis: Specific changes in the ECG, particularly in the ST segment, can indicate damage to parts of the heart muscle.
Structural Abnormalities: An ECG can hint at problems like an enlarged heart chamber.
Electrolyte Imbalances: Abnormal levels of potassium, calcium, or other ions in the bloodstream can impact the heart's electrical activity, evident in an ECG.
Effect of Medications: Some drugs can affect the heart's rhythm, and an ECG can help monitor these changes.
Types of ECG
Standard (Resting) ECG: The typical ECG where the patient is at rest during the test.
Holter Monitor: A portable ECG device worn for 24 to 48 hours, recording heart activity throughout daily routines.
Exercise (Stress) ECG: Performed while the patient is exercising, usually on a treadmill or stationary bike, to assess the heart's response to increased workload.
Event Recorder: A device worn for longer periods (weeks to months) that records only when certain heart rhythms are detected or when activated by the patient.
Challenges and Limitations
Artifact Interference: Muscle tremors, patient movement, or issues with the electrodes can produce "noise" in the ECG, making interpretation challenging.
Interpretation: ECGs require expert analysis, as subtle changes can be significant. Misinterpretation can lead to misdiagnosis.
Market Statistics:
Electrocardiograph The market was valued at $5.1 billion in 2020, and is expected to increase at a CAGR of 5.8% from 2021 to 2026. An electrocardiograph is a non-invasive test for checking and recording heart electrical activity.
Tags
Cardiology Conferences 2024
Cardiology Conferences 2024
Arrhythmia Conferences
Cardiology Conferences 2024
Cardiologist Conferences
Vascular Biology Conferences
Cardiac Imaging Conferences
Cardiac Nursing Conferences
Cardiology Conferences USA
Cardiology Conferences 2024 Australia
Stroke Conferences
Peers Alley Media Conferences
Cardio-Oncology: Bridging the Heart and Cancer Care
Cardio-oncology is an evolving interdisciplinary field that addresses the cardiovascular complications associated with cancer therapies. Given that advances in cancer treatment have led to improved survival rates, there has been an increased focus on the long-term side effects of these therapies, many of which have potential adverse impacts on the heart.
Genesis of Cardio-Oncology
As the efficacy of cancer treatments has grown, so too has the recognition of their side effects on the cardiovascular system. The field of cardio-oncology emerged from the need to:
Identify: Understand and recognize the cardiovascular complications linked to cancer therapies.
Prevent: Minimize the risk of heart diseases in cancer patients and survivors.
Manage: Treat cardiovascular diseases when they occur in this patient population.
Cardiovascular Complications of Cancer Therapies
Cancer treatments, while effective against malignancies, can lead to a spectrum of cardiovascular complications:
Chemotherapy-induced cardiomyopathy: Certain chemotherapy agents, like anthracyclines, can damage the heart muscle, leading to a decrease in heart function.
Arrhythmias: Abnormal heart rhythms can be induced by some cancer drugs.
Ischemic heart disease: Some therapies increase the risk of coronary artery disease or exacerbate existing conditions.
Hypertension: Elevated blood pressure is a frequent side effect of many cancer drugs.
Thromboembolic events: Increased risk of blood clots in veins or arteries.
Valvular heart disease: Some treatments can affect heart valves, leading to leakage or stiffening.
Radiation-induced heart disease: Radiation therapy to the chest can damage the heart and its associated structures.
Roles and Responsibilities in Cardio-Oncology
A cardio-oncologist plays several critical roles:
Risk Assessment: Before starting cancer treatment, evaluating patients for pre-existing heart diseases or risk factors.
Monitoring: Regularly checking heart function during cancer treatment, especially when high-risk therapies are used.
Intervention: Recommending modifications in cancer treatment or initiating cardiovascular treatments if heart issues are detected.
Education: Advising patients on heart-healthy behaviors and what symptoms to watch for.
Research: Engaging in studies to understand the cardiovascular implications of new and existing cancer treatments and develop strategies to mitigate risks.
The Future of Cardio-Oncology
The field is continually evolving with advancements in both cardiology and oncology. Emerging areas of interest include:
Personalized medicine: Tailoring cancer treatments based on individual cardiovascular risk profiles.
Biomarkers: Identifying molecules or genes that can predict cardiovascular risk in cancer patients.
New therapeutics: Developing heart-protective agents that can be co-administered with potentially cardiotoxic cancer drugs.
Tags
Cardiology Conferences 2024
Clinical Cardiology Conferences
Hypertension Conferences
Cardiology Conferences 2024
Heart Congress Japan
Cardiology Conferences 2024
Vascular Biology Conferences
Cardiology Conferences 2024 Australia
Cardiac Imaging Conferences
Cardiologist Conferences
Heart Conferences
Cardiology Conferences 2024 Canada
Cardiology Conferences 2024 Asia
Heart Diseases Conferences
Interventional Cardiology: Pioneering Minimally Invasive Heart Solutions
Interventional cardiology is a subspecialty within the broader field of cardiology that primarily deals with the catheter-based treatment of heart diseases. It focuses on using minimally invasive techniques to diagnose and treat a vast array of cardiovascular conditions, greatly reducing the need for traditional open-heart surgeries.
The Heart of Interventional Cardiology: The Catheter
Central to the procedures in interventional cardiology is the catheter—a thin, flexible tube that can be threaded through the blood vessels. Using advanced imaging techniques, physicians can guide the catheter to various parts of the heart, providing a means to both diagnose and treat heart conditions.
Common Procedures in Interventional Cardiology
Angioplasty (Percutaneous Coronary Intervention, PCI): This procedure involves inflating a small balloon inside a narrowed or blocked coronary artery to help widen it. Often, a stent (a small wire mesh tube) is placed to keep the artery open.
Catheter Ablation: Used to treat certain types of arrhythmias. It involves guiding a catheter to areas of the heart that are causing abnormal rhythms and then using energy (like radiofrequency) to destroy these tiny areas.
Valvuloplasty: A procedure where a balloon is inserted and inflated to widen a heart valve that has become narrowed.
Transcatheter Aortic Valve Replacement (TAVR): A minimally invasive procedure to replace a diseased aortic valve. It's especially beneficial for patients who are at high risk for traditional open-heart surgery.
Closure of Heart Defects: Devices can be delivered via catheter to close holes in the heart, such as atrial septal defects or patent foramen ovale.
Coronary Thrombectomy: A procedure to remove a blood clot from a coronary artery.
Advantages of Interventional Cardiology
Less Invasive: Compared to traditional surgeries, catheter-based procedures generally involve smaller incisions, reducing the risk of infection and complications.
Shorter Recovery Time: Patients often have shorter hospital stays and can return to normal activities sooner.
Reduced Pain and Discomfort: Minimally invasive procedures usually result in less post-operative pain.
Available to High-risk Patients: Some patients deemed too high-risk for traditional surgery may still be candidates for interventional procedures.
Challenges and Considerations
Complications: As with any medical procedure, there are risks, including bleeding, blood clots, or damage to the heart or blood vessels.
Long-term Outcomes: While many interventional cardiology procedures have excellent short-term outcomes, the long-term durability and effectiveness can vary based on the procedure and patient factors.
Emerging Innovations in Interventional Cardiology
The field is continuously advancing, with new techniques, devices, and technologies emerging regularly. Innovations include:
Drug-eluting stents: These stents release medications over time to prevent the artery from narrowing again.
Bioabsorbable stents: Stents that dissolve over time, leaving no permanent implant.
Robot-assisted procedures: Using robotic systems to enhance precision during catheter-based interventions.
Subtopics
Cardiac catheterization | Angioplasty | Coronary stents | Embolic protection | Percutaneous valve repair | Balloon valvuloplasty| Atherectomy
Market Statistics:
Due to COVID-19, the worldwide interventional cardiology market size is expected to be roughly $11.1 billion in 2020, down from over $14 billion in 2019. The global market is predicted to reach an astounding $16.2 billion in 2027.
Boston Scientific, Abbott, and Medtronic collectively held more than 40% of the global interventional cardiology market share.
As a result of COVID19, the worldwide interventional cardiology market size declined by 20% from 2019 to 2020, reaching a valuation of $11.1 billion in 2020.
Tags
Pediatric Cardiology Conferences
Heart Congress Japan
Stroke Conferences
Cardiology Conferences 2024
Cardiology Conferences USA
Clinical Cardiology Conferences
Heart Conferences
Arrhythmia Conferences
Cardiology Conferences 2024 Asia
Cardiology Conferences 2024
Hypertension Conferences
Cardiology Conferences 2024 Europe
Cardiac Imaging Conferences
Cardiology Conferences 2024
Cardiac Surgery Conferences
Nuclear cardiology is a medical speciality that focuses on the diagnosis and assessment of various cardiac problems using radioactive materials and advanced imaging techniques. It combines cardiology (the study of the heart and its functioning) and nuclear medicine (the use of radioactive substances to generate images and analyse biological processes). Nuclear cardiology is generally utilised to examine blood flow to the heart muscle as well as overall heart function.
The following are some important characteristics of nuclear cardiology:
1. Myocardial Perfusion Imaging (MPI): This is one of the most common nuclear cardiology tests. A small amount of a radioactive substance (such as technetium or thallium) is injected into the bloodstream. These radioactive tracers are taken up by the heart muscle in accordance to blood flow. Images of the tracer's distribution in the heart are then made using a specialized camera called a gamma camera. In order to diagnose coronary artery disease (CAD) and evaluate the severity of myocardial ischemia (insufficient blood flow to the heart muscle), MPI is useful.
2. Single Photon Emission Computed Tomography (SPECT): Nuclear imaging methods such as SPECT produce three-dimensional images of the heart. In order to evaluate blood flow to various parts of the heart, it is frequently used in conjunction with myocardial perfusion imaging.
3. Positron Emission Tomography (PET): Nuclear cardiology uses positron-emitting radionuclides, such as fluorodeoxyglucose (FDG), as a different type of radioactive tracer in PET scans. PET imaging is beneficial for detecting areas of the heart with lower metabolic activity, which may signify scar tissue from a previous heart attack, and can provide more detailed information regarding myocardial metabolism.
4. Cardiac Function Assessment: Nuclear cardiology can be used to evaluate the heart's general health as well as its efficiency in pumping blood. Techniques like equilibrium radionuclide angiography and gated blood pool imaging are used to accomplish this.
5. Viability Studies: These studies examine whether revascularization techniques, such as coronary artery bypass surgery or angioplasty, can still save or enhance certain regions of the heart that appear dysfunctional on imaging.
The diagnosis, risk assessment, and treatment of several of cardiac conditions, such as coronary artery disease, heart failure, and myocardial infarction (heart attacks), depend heavily on nuclear cardiology. Cardiologists and other medical professionals can use it to make informed decisions about patient care and treatment options.
Subtopics
Modern practices in cardiovascular therapy | Vasodilators | Percutaneous Coronary Intervention (PCI) | Heart Transplant| Application of cardiac progenitor cells | Imaging| Computed Tomography | Cardiac Magnetic Resonance | Nuclear Imaging | Molecular Imaging | Nuclear Cardiology | Hybrid and Fusion Imaging | Cross-Modality and Multi-Modality Imaging Topics
Market Statistics:
The nuclear medicine market is expected to grow at a 9.0 percent compound annual growth rate (CAGR) from USD 4.8 billion in 2021 to USD 7.5 billion in 2026.
This market is divided into four regions: North America, Europe, Asia-Pacific, and the Rest of the World. In terms of the nuclear cardiology market, North America has remained ahead of the other regions due to its superior capacity to handle new and highly advanced technologies.
Furthermore, new low-cost technologies like PET and PACS imaging technology will drive up demand for nuclear cardiology devices.
Tags
Peers Alley Media Conferences
Cardiology Conferences 2024
Cardiology Conferences USA
Heart Conferences
Cardiology Conferences 2024 Asia
Hypertension Conferences
Vascular Biology Conferences
Cardiology Conferences 2024 Canada
Arrhythmia Conferences
Cardiology Conferences 2024 Europe
Cardiologist Conferences
Pediatric Cardiology Conferences
Cardiac Imaging Conferences
Cardiology Conferences 2024 Australia
Heart Congress Japan
Care for patients with heart-related disorders and diseases are the primary objective of the specialized nursing specialty known as cardiac nursing. Assessment, monitoring, and management of patients with a range of cardiac conditions, including acute myocardial infarction (heart attack) and chronic heart conditions such congestive heart failure, are crucial roles for cardiac nurses.
Their responsibilities include:
1. Patient Assessment: Monitoring vital signs, performing physical examinations, and looking over medical histories are various methods that cardiac nurses evaluate patients' overall health and heart state. They hunt down heart issues' warning signals and symptoms. They search for indications and symptoms of heart issues.
2. Medication Administration: They administer medicines such as antiarrhythmics, anticoagulants, and vasodilators that doctors have prescribed. Patients are also informed about their drugs and their side effects by cardiac nurses.
3. Monitoring: In cardiac nursing, it is crucial to continuously monitor heart rhythms and vital signs. In order to identify changes in a patient's condition, cardiac nurses are frequently in charge of analyzing electrocardiograms (ECGs) and other diagnostic tests.
4. Education: A significant part of the job is educating patients and their families about heart disease prevention, lifestyle changes, and post-procedure care. They provide guidance on diet, exercise, and medication adherence.
5. Support during Procedures: Cardiac nurses may assist with a variety of cardiac procedures, including pacemaker installation, angioplasty, and cardiac catheterization. They make sure patients are ready for these treatments and offer post-procedure care.
6. Rehabilitation: Patients recovering from heart surgeries or heart attacks really must undergo cardiac rehabilitation. Cardiac nurses are involved in the planning and monitoring exercise programs, dietary changes, and stress reduce techniques.
7. Emergency Response: Code blue teams, which respond to cardiac emergencies in hospitals, frequently include cardiac nurses as members. They are trained how to utilize automated external defibrillators (AEDs) and perform cardiopulmonary resuscitation (CPR).
8. Assessment of Risk Factors: An essential aspect of cardiac nursing is recognizing and addressing risk factors for heart disease, such as high blood pressure, diabetes, and high cholesterol. They collaborate with patients to create risk-reduction strategies.
9. Collaboration: Cardiac nurses work closely with cardiologists, heart surgeons, and other healthcare professionals to develop and implement out a patient's treatment plan. They update the medical staff on changes in the patient's condition and progression.
10. Emotional Support: For patients and their families, dealing with heart disease can be extremely difficult. During the course of treatment and recovery, cardiac nurses offer emotional support, address concerns, and offer assurance.
Cardiac nursing is a dynamic discipline that needs continual education and training to stay up with improvements in cardiac care. Hospitals, cardiac care units, cardiac rehabilitation centers and outpatient clinics are just a few of the healthcare settings where nurses with this speciality may work. They are essential in enhancing the quality of life and assisting people with heart problems in efficiently managing their cardiac health.
Subtopics
Cardiac Diseases| Cardiac Surgery| Cardiac Nursing| Heart Diagnosis| Hypertension and Obesity| Stroke| Coronary artery disease| Cardiologists| Heart Regeneration| Angiography| Interventional Cardiology| Clinical Cardiology & Diabetes| Nursing Care| Cardiac Pharmacology| Case Reports on Cardiology| Clinical cardiac electrophysiology| Pediatric cardiology| Cardiac Research| Advanced Nursing
Market Statistics:
Salary for cardiovascular nurses varies depending on experience, region, and education level. These individuals earn an average base income of $88,646 each year. Total pay for cardiovascular nursing salary ranges from $51,000 to $90,000.
In general, the job prognosis for nurses is also positive. According to the Bureau of Labor Statistics, the number of registered nurses will increase by 7% between 2019 and 2029. With the ageing of the Baby Boomer generation and the prevalence of heart disease in the United States, the need for cardiovascular nurse employment is expected to rise.
Overall, the Bureau of Labor Statistics predicts that the registered nurse profession will grow by 7% between 2019 and 2029, which is good news for nurses of all specialties. Cardiovascular health is likewise a high-demand component of the healthcare system. According to the Centers for Disease Control and Prevention, heart disease is the leading cause of death in the United States, accounting for one out of every four deaths. In other words, there is still a demand for cardiovascular nursing employment in the sector.
Tags
Clinical Cardiology Conferences
Cardiac Surgery Conferences
Cardiology Conferences USA
Cardiology Conferences 2024 Asia
Heart Diseases Conferences
Cardiac Nursing Conferences
Heart Congress Japan
Heart Conferences
Cardiology Conferences 2024
Cardiac Imaging Conferences
Cardiology Conferences 2024 Australia
Cardiology Conferences 2024 Europe
Hypertension Conferences
Pediatric Cardiology Conferences
Cardiology Conferences 2024
The study of infants, children, adolescents, and young adults with heart problems and cardiovascular diseases is the focus of the medical discipline known as pediatric cardiology. Pediatric cardiologists are specifically trained doctors who are experts in treating young patients with cardiac problems.
Here are some key aspects of pediatric cardiology:
1. Diagnosis: To identify children's heart problems, pediatric cardiologists use a variety of tools and techniques. These could include physical examinations, cardiac catheterization, echocardiograms (heart ultrasounds), electrocardiograms (ECGs or EKGs), and other imaging studies.
2. Congenital Heart Disease: Congenital heart defects, or structural abnormalities in the heart, are present at birth in a large number of children. Pediatric cardiologists are skilled at diagnosing and treating these disorders, which can range from minor problems that don't need to be treated to complex, life-threatening defects.
3. Acquired Heart Conditions: Pediatric cardiologists also deal with acquired cardiac disorders that might appear in children, include myocarditis (heart muscle inflammation), Kawasaki illness, and certain arrhythmias (abnormal heart rhythms).
4. Treatment and Intervention: Treatment options can differ depending on the specific cardiac problem. Pediatric cardiologists may suggest medications, dietary modifications, interventional procedures (such as catheter-based interventions), or surgical procedures to treat or manage cardiac conditions.
5. Long-Term Care: In pediatric cardiology, children with cardiac disorders frequently require long-term management and follow-up care. This may entail keeping an eye on the child's development and growth, modifying the treatment plan as the child gets older, and providing continuous support to the child's family.
6. Collaboration: To provide complete care for kids with complex heart conditions, pediatric cardiologists frequently collaborate closely with other pediatric specialists, such as neonatologists, pediatric intensivists, and pediatric cardiothoracic surgeons.
7. Preventive Care: Pediatric cardiologists can help families learn about heart-healthy lifestyles and methods to prevent heart disease in children, especially when there is a family history of heart problems.
Overall, pediatric cardiology is a vital area of medicine that contributes to ensuring the health of kids with heart problems, from early diagnosis and treatment to continuous support and care throughout childhood and into adulthood.
Subtopics
Pediatrics| Clinical Pediatrics| Pediatric Cardiology| Pediatric Congenital Heart Disease| Pediatric Heart Murmurs| Cardiac Stroke| Fetal Cardiology| Pediatric Cardiac Tumors| Pediatric Kawasaki Disease| Pediatric Atherosclerosis| Tetralogy Of Fallot In Infants| Pediatric Pericarditis| Rheumatic heart disease| Pediatric Aortic Stenosis| Pediatric Pulmonary Atresia| Cardiac nursing| Pediatric Nursing
Market Statistics:
The worldwide paediatric interventional cardiology market is divided into two parts: device type and geography. The market is further divided into congenital heart defect closure devices, transcatheter heart valves, and others based on the kind of device (catheters, guidewires, balloons, and stents).
Interventional cardiology is a subspecialty of cardiology that treats coronary artery, valvular, and congenital heart disorders with intravascular catheter-based procedures and fluoroscopy. Pediatric interventional cardiology is the practise of performing interventional cardiology on newborns, children, and adolescents up to the age of 18.
St. Jude Medical (U.S.), Boston Scientific (U.S.), Gore Medical (U.S.), Abbott Vascular (U.S.), GE Healthcare (U.S.), Edward LifeSciences (U.S.) and Siemens Healthcare are among the market's major players (Germany).
Tags
Cardiology Conferences 2024 Asia
Cardiologist Conferences
Heart Congress Japan
Vascular Biology Conferences
Heart Conferences
Cardiology Conferences 2024
Heart Diseases Conferences
Cardiology Conferences 2024 Europe
Cardiac Surgery Conferences
Cardiology Conferences 2024
Pediatric Cardiology Conferences
Arrhythmia Conferences
Cardiology Conferences 2024 Australia
A stroke, often referred to as a cerebrovascular accident (CVA), is a dangerous medical condition that develops when there is an interruption in the blood flow to a part of the brain. Various reasons can cause this disruption, which prevents the brain from getting the nutrition and oxygen it requires to function normally. In turn, this can cause brain cells to become damaged or die, which can have a variety of long-term effects and neurological symptoms.
There are two main types of strokes:
1. Ischemic Stroke: With over 85% of all strokes falling within this category, it is the most common type of stroke. It happens when a blood vessel that supplies blood to the brain narrows or becomes blocked, frequently as a result of a blood clot. A blockage may arise from another the body, such as the heart (embolic stroke), or it may happen in the blood vessels of the brain (thrombotic stroke).
2. Hemorrhagic Stroke: This kind of stroke arises when a blood vessel in the brain bursts or leaks, resulting in bleeding into the surrounding brain tissue. Strokes that are hemorrhagic are more severe but less frequent than ischemic strokes. Hemorrhagic strokes can be classified into two primary subtypes: intracerebral hemorrhage (bleeding inside the brain) and subarachnoid hemorrhage (bleeding in the space between the brain and the skull).
The signs and symptoms of a stroke might vary depending on the part of the brain that is affected, but frequent ones include:
- Suddenly feeling weak or numb, frequently on one side of the body.
- Sudden difficulty speaking or confusion.
- A sudden visual issue, such as double or blurry vision.
- An unexpectedly severe headache.
- A sudden inability to walk, dizziness, loss of balance, or lack of coordination.
If a stroke is suspected, it is crucial to seek immediate medical assistance since prompt intervention can lessen brain damage and improve the outcome. To remember stroke warning symptoms, people frequently use the abbreviation FAST:
- F: Face drooping
- A: Arm weakness
- S: Speech difficulty
- T: Time to call emergency services
High blood pressure, smoking, diabetes, obesity, high cholesterol, a family history of stroke, and age (the risk rises with age) are all stroke risk factors. Rehabilitation and therapy can assist persons who have had a stroke recover from their symptoms, and lifestyle modifications and pharmacological interventions can prevent the chance of stroke.
Subtopics
Assessment of Stroke Patients | Stroke Etiology | Acute Stroke Imaging | Management of Stroke Patients | Stroke in Consultation | Prevention of First and Recurrent Stroke
Market Statistics:
The Global Stroke Management Market was worth $22,581 million in 2016 and is expected to be worth $36,756 million by 2023, expanding at a CAGR of 7.1 percent during the study period (2017-2023). Stroke is a medical emergency that occurs when blood flow to the brain is disrupted, causing brain cells to die.
The Stroke Management Market's Key Findings:
• The diagnostics sector dominated the market in 2016 and is expected to grow at the fastest CAGR of 8.1 percent in 2017.
• In 2016, the ischemic stroke category accounted for the largest share.
• In 2016, the United States was the largest shareholder in the North American stroke management market.
• During the analysis period, Asia-Pacific is predicted to have the highest growth rate.
• In the Asia-Pacific market, China is predicted to develop at the fastest CAGR.
Tags
Cardiologist Conferences
Cardiology Conferences USA
Clinical Cardiology Conferences
Cardiology Conferences 2024 Australia
Stroke Conferences
Peers Alley Media Conferences
Cardiac Nursing Conferences
Cardiology Conferences 2024 Asia
Cardiology Conferences 2024
Cardiac Surgery Conferences
Arrhythmia Conferences
Cardiology Conferences 2024
Cardiac surgery, commonly referred to as cardiovascular surgery, is a specialist area of surgery that is concerned with the treatment of conditions and diseases that affect the heart and blood vessels. Cardiac surgeons are skilled health care professionals who carry out surgical treatments to repair, replace, or modify the heart, blood vessels, and surrounding structures. These procedures are often carried out to improve the cardiovascular system's functioning and treat life-threatening illnesses or their symptoms.
The following are some common cardiac surgery procedures:
1. Coronary Artery Bypass Grafting (CABG): Coronary artery bypass grafting (CABG), often known as bypass surgery, is a treatment used to treat coronary artery disease (CAD). To bypass blocked or narrowed coronary arteries and improve blood flow to the heart muscle, surgeons extract a healthy blood vessel from another area of the body, typically the leg or chest.
2. Valve Surgery: Repairing or replacing damaged or defective heart valves is known as valve surgery. Stenosis (a constriction) and regurgitation (a leaking) are two disorders that can affect the heart valves. The valve can either be fixed surgically or replaced with a mechanical or bioprosthetic valve.
3. Aneurysm Repair: Aneurysms are abnormal bulges or weakness in blood vessels, and they can be dangerous if they occur in the aorta (the body's biggest artery). Aortic aneurysms can be replaced or repaired by cardiac surgeons, lowering the risk of rupture.
4. Congenital Heart Defect Repair: Congenital heart defects are heart abnormalities that some people have from birth. Corrective surgeries can be carried out by cardiac surgeons to fix these flaws and improve the heart's performance.
5. Arrhythmia Surgery: Surgery, such as the Maze procedure, can be used to generate scar tissue in the heart to disrupt abnormal electrical pathways and restore a normal heart rhythm in situations with severe arrhythmias (abnormal heart rhythms) that do not respond to other treatments.
6. Heart Transplantation: Heart transplantation may be the only option if the heart is severely damaged and cannot be repaired. The failing patient's heart is replaced with a healthy donor heart by cardiac surgeons working with transplant teams.
7. Left Ventricular Assist Device (LVAD) Placement: For a weak heart to pump blood more efficiently, mechanical devices called LVADs are implanted in the chest. When a patient is not a candidate for a heart transplant, they are frequently used as a bridge to heart transplantation or as a destination therapy.
8. Minimally Invasive Cardiac Surgery: Minimally invasive procedures have become more popular in heart surgery during the past few years. These procedures have a quicker recovery period and less scarring since they use small incisions and use specialized instruments.
A highly qualified and specialized team, including cardiac surgeons, anesthesiologists, nurses, and other medical professionals, is needed for the complex and delicate field of cardiac surgery. It is frequently carried out in hospitals with specialized heart surgery units or cardiac surgery centers.
In order to decide the most appropriate plan of treatment for their specific condition, patients often go through a thorough evaluation before having cardiac surgery. The patient's diagnosis, overall health, and unique circumstances all play a role in the surgical technique selection. The results and quality of life for many people with heart conditions have improved as a result of considerable advancements in cardiac surgery over time.
Subtopics
Perioperative Management | Surgery for ischemic Heart Disease | Surgery for Valvular Heart Disease | Surgery for Heart Failure | Thoracic Aortic Disease | Surgery for Cardiac Rhythm Disorders and Tumors | Surgery for Congenital Heart Disease
Market Statistics:
The global market for cardiac surgical instruments is predicted to reach USD 1.63 billion by 2022, up from USD 1.16 billion in 2017, at a CAGR of 7.1%.
Europe dominated the global market in 2017, followed by North America. The European market is primarily driven by increased use of surgical treatments in cardiology, expansion in the European healthcare sector, and public awareness campaigns. The Asian market, on the other hand, is expected to grow at the fastest CAGR due to increased government and private sector spending in healthcare, rising purchasing power, and a high prevalence of cardiac disorders. China, India, and Japan are three of Asia's most important marketplaces.
Tags
Clinical Cardiology Conferences
Cardiology Conferences 2024 Europe
Pediatric Cardiology Conferences
Hypertension Conferences
Cardiology Conferences 2024 Canada
Stroke Conferences
Cardiology Conferences 2024
Heart Diseases Conferences
Vascular Biology Conferences
Heart Conferences
Cardiology Conferences USA
Cardiology Conferences 2024
Cardiac Imaging Conferences
The medical condition known as thrombosis is defined by the formation of a blood clot (thrombus) within a blood vessel, which can block blood flow. Depending on where it forms and how big it is, this clot may form in veins or arteries all over the body and may have significant effects.
The two main categories of thrombosis are:
1. Venous Thrombosis: This occurs when a blood clot forms in a vein, commonly in the pelvic, arm, or deep veins of the legs (deep vein thrombosis, or DVT). A pulmonary embolism, a potentially fatal illness, can result from DVT if the blood clot escapes and travels through the bloodstream to the lungs.
2. Arterial Thrombosis: This happens when a blood clot forms in an artery, which can result in the restriction of blood flow to vital organs or tissues. When it affects the coronary arteries that supply the heart or brain, arterial thrombosis can lead to serious conditions like heart attacks (myocardial infarction) or strokes (cerebral thrombosis or embolism).
The development of thrombosis can be caused by a number of factors, such as:
- Damage or injury to the blood vessel walls.
– Changes in blood flow patterns.
- Hypercoagulability, a term used to describe a blood's increased tendency to clot.
Genetics, age, obesity, immobility (such as prolonged time spent in bed or on long flights), surgery, pregnancy, hormone therapy, certain medical conditions (including cancer), and a history of prior thrombotic events are risk factors for thrombosis.
Anticoagulant drugs (blood thinners) are frequently used in the treatment of thrombosis to stop the clot from getting bigger and to lower the risk of further clot formation. To dissolve or remove the clot in some circumstances, more invasive procedures may be required. The location and severity of the thrombosis, as well as the patient's general condition, determine the best course of treatment. It may also be advised to take preventative steps, such as medication and lifestyle modifications, to lower the risk of future thrombotic events, particularly in people who have underlying risk factors.
Subtopics
Hemostasis and Thrombosis | Coagulation and Its Regulation | Fibrinolysis and Its Regulation | Platelet Structure and Function | Thrombohemorrhagic Disorders | Therapy, New Directions and Complications in Thrombohemorrhagic Disorders
Tags
Cardiac Imaging Conferences
Cardiac Nursing Conferences
Heart Congress Japan
Cardiology Conferences 2024 Asia
Cardiology Conferences USA
Clinical Cardiology Conferences
Hypertension Conferences
Cardiology Conferences 2024 Canada
Pediatric Cardiology Conferences
Cardiac Surgery Conferences
Cardiology Conferences 2024
Heart Conferences
Heart Diseases Conferences
Cardiology Conferences 2024 Europe
Arrhythmia Conferences
An irregular heartbeat or abnormal cardiac rhythm is referred to as heart arrhythmia, or simply arrhythmia. To effectively pump blood throughout the body, the heart normally beats in a regular, coordinated manner. The sinoatrial (SA) node, the heart's natural pacemaker, generates electrical signals that pass through the electrical conduction system of the heart to regulate this rhythmic beating.
These electrical signals may be disrupted with in the case of arrhythmia, resulting in a number of irregular cardiac rhythms.
Arrhythmias can be divided into several categories, including:
Subtopics
Sinus node: Normal and Abnormal Rhythms | Bradyarrhythmias | Ectopic Complexes and Rhythms | Tachycardia | Supraventricular Tachyarrhythmias | Ventricular Tachyarrhythmias | Cardiac Pacing and Pacemaker Rhythms | Implantable Cardioverter Defibrillators | Athletes and Arrhythmias | Drug Effects and Electrolyte Disorders | Treatment of Arrhythmias | Management of Arrhythmias in Pregnancy
Tags
Cardiology Conferences 2024
Cardiology Conferences 2024
Cardiology Conferences 2024 Australia
Cardiology Conferences USA
Heart Conferences
Hypertension Conferences
Arrhythmia Conferences
Stroke Conferences
Cardiology Conferences 2024 Asia
Pediatric Cardiology Conferences
Cardiology Conferences 2024 Canada
Cardiac Imaging Conferences
Peers Alley Media Conferences
Cardiac Nursing Conferences
Valvular heart disease (VHD) is a medical condition that affects the heart's valves. The aortic valve, pulmonary valve, tricuspid valve, and mitral valve are the four valves that make up the heart. These valves are essential in ensuring that blood flows through the heart chambers in one direction. When one or more of these valves are damaged or dysfunctional, the heart's blood flow is distorted and valvular heart disease develops.
Valvular heart disease can be divided into two categories:
The following list of factors can cause valvular heart disease:
The diagnosis typically involves a combination of physical examination, imaging tests (such as echocardiography), and occasionally cardiac catheterization to evaluate the severity of valve disease and choose the most appropriate course of action.
Depending on how severe the problem is, there are several treatment options available, including:
To properly treat their condition and avoid complications, people with valvular heart disease require routine follow-up care and monitoring. Depending on the patient's specific condition and needs, treatment recommendations should be made in consulation with a cardiologist or a cardiac surgeon.
Subtopics
Epidemiology of Valvular Heart Disease | Cellular and Molecular Basis of Calcific Aortic Valve Disease | Clinical and Genetic Risk Factors for Calcific Valve Disease | Evaluation of Valvular Heart Disease by Cardiac Magnetic Resonance and Computed Tomography | Aortic Stenosis | Aortic Regurgitation | Aortic Valve Implantation | Surgical Approach to Diseases of the Aortic Valve | Rheumatic Mitral Valve | Myxomatous Mitral Valve | Infective Endocarditis | Prosthetic Heart Valves | Valvular Heart Disease in Pregnancy
Tags
Cardiology Conferences 2024
Arrhythmia Conferences
Cardiology Conferences 2024 Australia
Cardiac Imaging Conferences
Cardiology Conferences 2024
Heart Congress Japan
Hypertension Conferences
Cardiology Conferences 2024 Asia
Cardiology Conferences 2024 Europe
Cardiologist Conferences
Cardiology Conferences 2024 Canada
Cardiac Surgery Conferences
Peers Alley Media Conferences
Vascular Biology Conferences
Heart Diseases Conferences
"Advances in Non-Invasive Cardiac Imaging Techniques" describes the progress and innovations made in medical imaging techniques that enable healthcare professionals to evaluate the structure and function of the heart without invasive procedures like surgery or catheterization. These techniques are essential for the evaluation and monitoring of several cardiac conditions, including congenital heart defects, heart failure, and coronary artery disease as well as heart valve problems.
The following are a few of the most important non-invasive cardiac imaging techniques:
Tags
Heart Diseases Conferences
Cardiology Conferences 2024 Europe
Cardiology Conferences USA
Heart Conferences
Pediatric Cardiology Conferences
Heart Congress Japan
Cardiology Conferences 2024
Cardiology Conferences 2024 Asia
Vascular Biology Conferences
Cardiology Conferences 2024 Canada
Clinical Cardiology Conferences
Cardiac Surgery Conferences
Cardiology Conferences 2024
By providing patients easy access to medical professionals and enabling continuous cardiac health monitoring, telemedicine and remote monitoring have changed the field of cardiac care.
Here is a summary of how remote monitoring and telemedicine are utilized in cardiac care:
1. Telemedicine Consultations: Patients can make virtual appointments with cardiologists and other medical professionals through telemedicine. Patients can talk about their symptoms, review test results, and get treatment advice during these sessions. As a result, fewer in-person visits are required, especially for follow-up appointments and routine checkups.
2. Remote Monitoring Devices: A remote monitoring device is used to continuously monitor a patient's heart condition.
Typical devices consist of:
3. Home Blood Pressure Monitoring: A major risk factor for heart disease is high blood pressure. Patients can use telemedicine platforms to monitor their blood pressure at home and communicate the results with their healthcare providers.
4. Medication Management: Through telemedicine, a patient's medication plans can be reviewed, dosages can be changed as necessary, and adherence can be checked.
5. Diet and Lifestyle Counseling: Cardiovascular care often involves dietary adjustments and increased physical exercise. Telemedicine enables continuous guidance and assistance in these areas.
6. Education and Support: Telemedicine platforms can offer patients educational resources and support services to help patients understand their condition, treat their symptoms, and make decisions about their cardiac health.
Benefits of Remote Monitoring and Telemedicine in Cardiac Care:
Tags
Clinical Cardiology Conferences
Cardiology Conferences 2024 Europe
Cardiologist Conferences
Cardiology Conferences 2024 Asia
Pediatric Cardiology Conferences
Cardiology Conferences 2024
Peers Alley Media Conferences
Cardiac Surgery Conferences
Heart Congress Japan
Vascular Biology Conferences
Cardiology Conferences 2024 Australia
Cardiac Nursing Conferences
Hypertension Conferences
Cardiology Conferences 2024
Cardiac Imaging Conferences
With the introduction of 3D and 4D (three-dimensional and four-dimensional) imaging technology, cardiac imaging has significantly advanced in recent years. These advancements have completely changed how medical practitioners now diagnose, monitor, and treat a variety of cardiac conditions.
Here's an overview of the impact of 3D and 4D cardiac imaging in the field of cardiology:
Tags
Cardiology Conferences USA
Cardiac Surgery Conferences
Heart Diseases Conferences
Cardiology Conferences 2024 Europe
Stroke Conferences
Cardiology Conferences 2024 Canada
Vascular Biology Conferences
Clinical Cardiology Conferences
Pediatric Cardiology Conferences
Cardiac Imaging Conferences
Cardiology Conferences 2024
Cardiologist Conferences
Cardiology Conferences 2024 Asia
Heart Congress Japan
Cardiac Nursing Conferences
Stem cell therapy for cardiac regeneration is a promising field of research and potential treatment for heart diseases. It involves using stem cells to repair damaged cardiac tissue and enhance the heart's functionality.
Here is a summary of this therapy's operation current state:
1. Stem Cells: Stem cells are unique cells that have the ability to develop into various cell types in the body. They can be obtained from a variety of sources, including adult stem cells, induced pluripotent stem cells (iPSCs), and embryonic stem cells.
2. Types of Stem Cells Used:
3. Mechanism of Action: When stem cells are introduced into the injured cardiac tissue, they may potentially differentiate into Functional cardiomyocytes and other supportive cells. Additionally, they may secrete factors that lessen inflammation and promote angiogenesis (formation of new blood vessels), which both help in tissue repair.
4. Delivery Methods: A variety of techniques can be used to deliver stem cells to the heart, including intravenous injection, direct injection into the heart tissue, and the use of specialized delivery systems, such as patches or scaffolds.
5. Current Status: In preclinical research and some early clinical trials, stem cell therapy for cardiac regeneration has showed promise. It is still a developing field, so there are a number of difficulties to overcome:
Tags
Cardiology Conferences 2024 Europe
Arrhythmia Conferences
Cardiac Imaging Conferences
Heart Diseases Conferences
Stroke Conferences
Heart Congress Japan
Hypertension Conferences
Clinical Cardiology Conferences
Heart Conferences
Cardiac Nursing Conferences
Cardiologist Conferences
Cardiology Conferences 2024
Cardiology Conferences 2024
Cardiac Surgery Conferences

Cardiac arrhythmias are irregular cardiac rhythms that can range from harmless to life threatening. They can be caused by a number of genetic and non-genetic factors. This response will concentrate on the genetics of cardiac arrhythmias.
Tags
Pediatric Cardiology Conferences
Cardiology Conferences 2024 Europe
Heart Conferences
Cardiology Conferences USA
Cardiac Imaging Conferences
Cardiac Nursing Conferences
Cardiology Conferences 2024 Asia
Heart Diseases Conferences
Cardiology Conferences 2024 Australia
Vascular Biology Conferences
Clinical Cardiology Conferences
Cardiologist Conferences
Hypertension Conferences
Heart Congress Japan
Cardiology Conferences 2024 Canada
Cardiovascular disease (CVD) is a broad term that refers to a variety of conditions that affect the heart and blood vessels. Conditions such as coronary artery disease, heart failure, stroke, and peripheral artery disease are included. While both men and women are affected by CVD, there are significant differences in how it manifests and is managed in women.
Here are some important aspects to consider when it comes to cardiovascular disease in women:
Tags
Stroke Conferences
Cardiology Conferences 2024 Europe
Heart Diseases Conferences
Heart Congress Japan
Peers Alley Media Conferences
Pediatric Cardiology Conferences
Cardiac Imaging Conferences
Cardiac Surgery Conferences
Clinical Cardiology Conferences
Cardiologist Conferences
Cardiology Conferences 2024
Arrhythmia Conferences
Cardiology Conferences 2024 Asia

Cardiac biomaterials and tissue engineering are interdisciplinary fields that attempt to create innovative therapies for cardiovascular diseases and repair damaged heart tissues. These fields of study combine principles from materials science, biology, and engineering to develop biomaterials and tissue constructs that can replace or heal damaged heart tissue, improve cardiac function, and, eventually, improve the quality of life for people with heart disorders.
Here are some of the most important components of cardiac biomaterials and tissue engineering:
Tags
Cardiac Imaging Conferences
Clinical Cardiology Conferences
Cardiology Conferences 2024
Cardiology Conferences 2024 Canada
Pediatric Cardiology Conferences
Peers Alley Media Conferences
Cardiology Conferences 2024 Australia
Cardiac Surgery Conferences
Cardiology Conferences USA
Arrhythmia Conferences
Vascular Biology Conferences
Cardiology Conferences 2024 Asia
Heart Diseases Conferences
Hypertension Conferences
Several innovations in cardiology education and training have occurred in recent years, with the goal of improving the skills and knowledge of healthcare professionals in the field. These innovations are motivated by the need to keep up with cardiology advancements, improve patient care, and address the growing burden of cardiovascular diseases.
The following are some important developments and innovations in cardiac education and training:
Tags
Pediatric Cardiology Conferences
Cardiology Conferences 2024
Vascular Biology Conferences
Hypertension Conferences
Cardiac Surgery Conferences
Cardiology Conferences 2024 Asia
Heart Conferences
Cardiology Conferences 2024
Heart Diseases Conferences
Cardiology Conferences 2024
Stroke Conferences
Clinical Cardiology Conferences
Precision medicine in cardiology is a customized approach for diagnosing, treating, and preventing cardiovascular diseases (CVD) that takes into account each person's particular genetic, molecular, environmental, and lifestyle factors. With this strategy, the effectiveness of interventions and therapies is maximized while adverse effects are reduced.
Key elements of precision medicine in cardiology include the following:
Tags
Heart Conferences
Cardiologist Conferences
Cardiology Conferences 2024
Cardiology Conferences 2024 Australia
Heart Congress Japan
Cardiology Conferences 2024 Canada
Cardiac Imaging Conferences
Hypertension Conferences
Pediatric Cardiology Conferences
Cardiology Conferences USA
Cardiology Conferences 2024
Stroke Conferences
Peers Alley Media Conferences
Heart Diseases Conferences
Artificial intelligence (AI) has made significant strides in various fields of medicine, including cardiovascular medicine. In this area, artificial intelligence (AI) applications are being used to enhance patient care, diagnosis, risk assessment, and treatment plans.
Here are some significant applications of AI in cardiology:
1. Diagnosis and Risk Assessment:
2. Treatment Planning and Decision Support:
3. Remote monitoring and telehealth:
4. Predictive analytics:
5. Research and Drug Discovery:
6. Patient Risk Stratification:
Tags
Heart Congress Japan
Arrhythmia Conferences
Pediatric Cardiology Conferences
Hypertension Conferences
Cardiac Imaging Conferences
Cardiologist Conferences
Cardiology Conferences 2024 Asia
Cardiology Conferences 2024
Heart Conferences
Cardiac Nursing Conferences
Cardiology Conferences 2024 Canada
Cardiology Conferences 2024 Australia
Vascular Biology Conferences
Cardiology Conferences 2024 Europe
Stroke Conferences
Cardiology and pulmonology are two separate medical specialities that concentrate on various parts of the human body, particularly the respiratory and cardiovascular systems.
An summary of each specialty is given below:
1. Pulmonology:
2. Cardiology:
Subtopics
Allergic bronchopulmonary aspergillosis | Asthma | Chronic obstructive pulmonary disease | Chronic bronchitis | Emphysema | Cystic fibrosis | Lung canceriagnosis | Pneumoconiosis | Pneumonia | Pneumothorax | Psittacosis | Pulmonary embolism | Pulmonary fibrosis | Pulmonary hypertension | Pulmonary sequestration | Sarcoidosis | Sleep apnea | Tuberculosis | Internal medicine | Intensive care medicine.
Tags
Vascular Biology Conferences
Cardiology Conferences USA
Pediatric Cardiology Conferences
Arrhythmia Conferences
Cardiac Imaging Conferences
Peers Alley Media Conferences
Cardiology Conferences 2024 Australia
Stroke Conferences
Heart Congress Japan
Hypertension Conferences
Cardiology Conferences 2024 Canada
Cardiology Conferences 2024
Heart Conferences
Cardiac Nursing Conferences
The condition known as atherosclerosis results from the buildup of fatty deposits, cholesterol, calcium, and other chemicals on the inner walls of the arteries, which causes the arteries to narrow and stiffen. The word "plaque" is used to characterize this collection. As the plaque accumulates and hardens, blood flow through the affected arteries may become reduced over time.
Here's how atherosclerosis typically develops:
Subtopics
Pathogenesis of Atherosclerosis | Chemokines and Atherosclerosis: A critical Assessment of Therapeutic Targets | Adhesion Molecules and Atherosclerosis | Cytokines and Atherosclerosis | Toll-Like Receptors in Atherosclerosis| PPAR-Based Therapies for the Management of Atherosclerosis | Pentraxins in Vascular Pathology | Metalloproteinase, the Endothelium and Atherosclerosis | Cathepsins in Atherosclerosis | The Plasmin system and Atherosclerosis | Mast Cell Proteases and Atherosclerosis | NADPH Oxidase and Atherosclerosis | Hene Oxygenase-1 and Atherosclerosis | Platelets: Role in Atherogenesis and thrombosis in Coronary Artery Disease
Tags
Hypertension Conferences
Vascular Biology Conferences
Heart Conferences
Cardiac Imaging Conferences
Cardiology Conferences 2024 Australia
Clinical Cardiology Conferences
Cardiac Surgery Conferences
Cardiac Nursing Conferences
Cardiologist Conferences
Arrhythmia Conferences
Cardiology Conferences 2024
Pediatric Cardiology Conferences
Cardiology Conferences 2024
Peers Alley Media Conferences
The cardiovascular health of athletes and people who regularly engage in physical exercise, particularly at competitive levels, is the focus of the specialist medical discipline known as sports cardiology.
Cardiology (the study of heart illnesses) and sports medicine (the study of injuries and health issues related to exercise and sport) are both incorporated into it. The major goal of sports cardiology is to assess and treat athletes' cardiovascular health in order to maintain their safety and maximize performance.
Aspects of sports cardiology include the following:
Subtopics
Athlete's Heart | Electrocardiography in athletes | Radionuclide Scintigraphy in athletes | Athlete's bradycardia | Exercise in healthy subjects| Exercise in cardiovascular disease | Sports and Hypertension| Exercise and sports in congenital heart disease | Sports and cardiovascular disease | Sudden cardiac death in sports | Accurate diagnosis and treatment plans | Frequency and causes of SCA in young athletes | Cardiovascular assessment
Tags
Heart Congress Japan
Heart Conferences
Cardiology Conferences 2024 Europe
Cardiac Imaging Conferences
Hypertension Conferences
Cardiology Conferences 2024
Stroke Conferences
Heart Diseases Conferences
Cardiology Conferences 2024 Asia
Cardiology Conferences 2024
Cardiologist Conferences
Cardiology Conferences USA
Pediatric Cardiology Conferences
Clinical Cardiology Conferences
Cardiology Conferences 2024
Cardiac imaging is a medical field that involves the use of various imaging techniques to visualize and assess the structure and function of the heart. For the diagnosis and continual monitoring of heart related issues and conditions, these methods are crucial. Heart-related imaging techniques come in a variety of forms, each with unique benefits and applications.
Cardiovascular imaging methods that are often used include:
Subtopics
Ischemic Heart Disease| Heart Failure| Acquired Valvular Heart Diseases| Cardiomyopthy | Cadiovascular Computed Tomography| Cadiovascular Magnetic Resonance| Great Vessel Abnormalities| Congenital Heart Disease| Coronary Artery Variant and Anomalies| Coronary Artery Disease| Myocardial Disease-Ischemia and Infraction| Myocardial Disease- Cardiomyopathy| Myocardial Disease- Masses| Cardiac Valvular Disease| Pericardial Disease| Postintervention/Postoperative
Market Statistics:
The global market for Heart Imaging, which was valued at US$14.8 billion in 2020, is expected to reach a revised size of US$27.5 billion by 2027, rising at a CAGR of 9.3% between 2020 and 2027.
The market for structural heart imaging in the United States is expected to be worth $4 billion by 2020. China, the world's second largest economy, is expected to reach a projected market size of US$5.8 billion by 2027, with a CAGR of 12.3% from 2020 to 2027. Other notable geographic markets include Japan and Canada, which are expected to increase at 6.3% and 7.9%, respectively, between 2020 and 2027. Germany is expected to expand at a CAGR of about 7.2% in Europe.
Asia-Pacific is expected to reach US$3.9 billion by 2027, led by countries such as Australia, India, and South Korea, while Latin America will grow at a 9.4% CAGR during the analysis period.
Tags
Arrhythmia Conferences
Pediatric Cardiology Conferences
Cardiology Conferences USA
Cardiac Surgery Conferences
Peers Alley Media Conferences
Cardiac Imaging Conferences
Clinical Cardiology Conferences
Hypertension Conferences
Cardiology Conferences 2024 Europe
Heart Diseases Conferences
Heart Conferences
Heart Congress Japan
Vascular Biology Conferences
Cardiology Conferences 2024
Vascular biology is a branch of biology that focuses on the study of blood vessels, also known as the vascular system. The structure, function, and regulation of blood vessels, including arteries, veins, and capillaries, are all issues covered by this field. The vascular system, which is in charge of transporting blood, nutrients, oxygen, and hormones to various tissues and organs, is essential for maintaining the overall health and functionality of the human body.
Important fields of research in vascular biology include:
Subtopics
Physiology of Blood vessels | Immunology of the vessel wall | Biology of thee vasculature | The endothelial cell | Vascular smooth muscle cells | Arteriogenesis Vs Angiogenesis | The lymphatic system | Pathogenesis of atherosclerosis | Atherosclerosis | Molecular Mechanisms | Pathophysiology of other cardiovascular diseases | Valvular heart diseases | Pathophysiology of thrombosis | Vascular pathophysiology of hypertension
Market Statistics:
The global vascular grafts market was worth USD 1.6 billion in 2020, and it is predicted to increase at a CAGR of 6.8% between 2021 and 2028. The rising prevalence of cardiovascular illnesses, diabetes, and end-stage renal disease are all propelling the market. According to the American Heart Association, an estimated 121.5 million people in the United States suffer from cardiovascular disorders such as high blood pressure, chest pain, heart attack, and stroke.
Tags
Cardiac Surgery Conferences
Heart Conferences
Cardiac Nursing Conferences
Stroke Conferences
Heart Diseases Conferences
Cardiac Imaging Conferences
Cardiology Conferences 2024
Pediatric Cardiology Conferences
Clinical Cardiology Conferences
Cardiology Conferences USA
Vascular Biology Conferences
A case report in medicine is a comprehensive report of an individual patient's signs, symptoms, diagnosis, treatment, management and follow-up. For science, medical and educational purposes, case reports can be circulated.
For medical-clinical research, evidence-based medicine, a case report plays a vital role and offers a case-based learning framework.
Case studies on cardiology are intended for: • Learning about medical cases or patients with heart problems offers valuable experience for cardiologists, physicians and paramedic personnel • Learning different diagnostic procedures from various medical cases• Positive and negative results, demographic profile of patients, tests and inquiries, including clinical photos, should be included in the case report.
Subtopics
Case Reports on Heart Disease & Failure | Case Reports on Vascular Heart Disease | Case Reports on Myocardial and Pericardial Disease | Case Reports on Pediatric Cardiology | Case Reports on Arrhythmias | Case Reports on Atherosclerosis | Case Reports on Hypertension and Healthcare | Case Reports on Heart Regeneration | Case Reports on Cardiac and Cardiovascular Research | Case Reports on Heart Diagnosis | Case Reports on Heart Devices | Case Reports on Cardiac Surgery | Case Reports on Cardiology - Future Medicine
Tags
Vascular Biology Conferences
Cardiology Conferences 2024
Cardiology Conferences 2024 Canada
Stroke Conferences
Cardiology Conferences 2024 Europe
Peers Alley Media Conferences
Cardiology Conferences 2024
Pediatric Cardiology Conferences
Cardiac Nursing Conferences
Arrhythmia Conferences
Cardiac Imaging Conferences
Heart Diseases Conferences
Heart Congress Japan
Cardiology Conferences 2024 Australia
Cardiology Conferences USA
Geriatric cardiology is a subspecialty of cardiology that focuses on the diagnosis, treatment, and prevention of cardiovascular disorders in older people, typically those who are 65 years of age and older. Geriatric cardiology covers these particular issues and challenges since older persons are more vulnerable to various cardiovascular problems.
Geriatric cardiology's salient features include the following:
Subtopics
Cardiology | Geriatrics | Elderly care | Heart diseases | Atherosclerosis | Peripheral arterial disease
Market Statistics:
In 2015, the global geriatric medication market was worth roughly USD 540 billion. The fast growing geriatric population base is one of the primary elements contributing to its rapid expansion. The worldwide geriatric population was estimated to be approximately 809.4 million in 2012, according to UN estimations, and is expected to reach almost 1.13 billion by 2022, and exceed a value of over 2 billion by 2050.
The growing elderly population in the world, as well as the increasing incidence of cardiovascular illnesses, are two of the most important aspects driving market revenue growth.
A new report from Emergen Research estimates that the global interventional cardiology devices market had a value of USD 13.72 billion in 2020 and is predicted to grow to USD 26.84 billion in 2028, with a revenue compound annual growth rate of 8.7 percent over the forecast period of 2021-2028.
Tags
Heart Diseases Conferences
Pediatric Cardiology Conferences
Clinical Cardiology Conferences
Hypertension Conferences
Stroke Conferences
Cardiology Conferences 2024
Arrhythmia Conferences
Cardiology Conferences 2024 Canada
Cardiac Imaging Conferences
Cardiologist Conferences
Cardiac Surgery Conferences
Heart Congress Japan
Cardiology Conferences 2024
Cardiology Conferences 2024
Cardiology Conferences 2024 Asia
Cardiovascular pharmacology is a branch of pharmacology that focuses on the study of drugs and medications used to treat conditions related to the cardiovascular system, which includes the heart and blood vessels. This topic is important because drugs play a big part in managing and preventing cardiovascular illnesses, which are among the major causes of death in the world.
The following are important topics in cardiovascular pharmacology:
Subtopics
The Cardiovascular Physiology and Pharmacology of Endothelin-I | Vascular Pharmacology of Epoxyeicosatrienoic Acids | Prostaglandins in Action | TP Receptors and Oxidative Stress | Regulation of Endothelial Cell Tetrahydrobiopterin | Polyphenol-Induced Endothelium-Dependent Relaxations | Organic Nitrates and Nitrate Tolerance | Vascular Actions of Adipokines | Cardiovascular Effects of Erythropoietin
Market Statistics:
By 2022, the global cardiovascular medicines market is expected to have grown from $141.1 billion in 2017 to $149.4 billion, representing a compound annual growth rate (CAGR) of 1.2 percent between 2017 and 2022.
Cardiovascular illnesses are one of the most common causes of death throughout the world. Following the American Heart Association's estimates, around 41.5 percent of the United States' population was suffering from some type of cardiovascular disease in 2015. This prevalence is expected to rise to 45 percent by 2035, according to the American Heart Association. Patients suffering from cardiovascular diseases are projected to increase in number as a result of a more sedentary lifestyle, shifting food habits, and an increase in risk factors.
Tags
Cardiology Conferences 2024 Europe
Heart Congress Japan
Peers Alley Media Conferences
Cardiac Surgery Conferences
Cardiologist Conferences
Cardiology Conferences USA
Cardiology Conferences 2024
Cardiology Conferences 2024
Pediatric Cardiology Conferences
Heart Conferences
Hypertension Conferences
Cardiac Nursing Conferences
Cardiology Conferences 2024 Australia
Cardiology Conferences 2024 Canada
Arrhythmia Conferences
Robotic cardiac surgery, often referred to as robot-assisted cardiac surgery or robotically-assisted cardiac surgery, is a minimally invasive surgical technique used to carry out heart operations with the aid of robotic systems. In comparison to conventional open-heart surgery, this cutting-edge technology enables cardiac surgeons to operate with more control and precision, potentially improving patient outcomes.
The following are some essential elements of robotic cardiac surgery:
Subtopics
Anesthesia for Robotic Cardiac Surgery | Robotic Mitral Valve Surgery | Robotic Coronary Bypass Graft on Beating Heart | Robotic Surgery in Congenital Heart Disease | Intraoperative Transesophageal Echocardiography | Hybrid coronary revascularization | Robotic Left Ventricular Epicardial Lead Implantation
Market Statistics:
The need for heart surgery is increasing over the world. During the period 2017-2025, robots will have a cumulative market value of $7.50 billion, owing to the large increase in the number of robot-based and computer-assisted cardiological surgery procedures for the treatment of heart problems.
According to industry estimates, the global surgical robots market is estimated to reach USD 6.4 billion in 2021 and to increase at a compound annual growth rate (CAGR) of 17.6 percent from 2021 to 2026. Surgical robots allow surgeons to perform complex surgical procedures with greater precision.
Tags
Cardiology Conferences 2024 Asia
Cardiology Conferences 2024 Canada
Stroke Conferences
Cardiologist Conferences
Cardiology Conferences 2024
Cardiology Conferences 2024 Europe
Peers Alley Media Conferences
Cardiac Nursing Conferences
Cardiology Conferences 2024 Australia
Pediatric Cardiology Conferences
Hypertension Conferences
Arrhythmia Conferences
Clinical Cardiology Conferences
Cardiology Conferences 2024
Heart Diseases Conferences
The process of repairing and replacing damaged or injured cardiac (heart) tissue is referred to as cardiac regeneration. Cardiomyocytes are specialized muscle cells that make up the heart, a crucial organ. It can be challenging for these cardiomyocytes to spontaneously regenerate when they are injured due to conditions like heart attacks (myocardial infarctions) or other heart illnesses because the adult heart has less ability for regeneration than some other tissues in the body.
However, cardiac regeneration is a topic of continuous study and attention as a potential therapeutic strategy to restore heart function. In the area of cardiac regeneration, a number of strategies and techniques are being researched, including:
Subtopics
Cell Based Heart Repair | Progenitor Cells from the Adult Heart | Human Pluripotent Stem Cell-Derived Cardiomyocytes | Direct Cardiac Reprogramming | Cardiomyocyte Transplantation | Tissue Engineered Heart repair | Imaging Cardiac Stem Cell Therapy | Stem Cell Transplant Immunology | Tissue graft cardiac cell replacement | Cardiac remodeling | Cardiac regenerative therapy | Congenital heart disease and regeneration | Heart repair, heart tissue regeneration and stem cells | Biomimetic heart valve replacement | Stem cell-derived engineered cardiac tissue
Market Statistics:
The global regenerative medicine market was estimated at USD 27.29 billion in 2020, and it is predicted to increase at a CAGR of 11.27% from 2021 to 2027.
Tags
Cardiology Conferences 2024 Canada
Cardiology Conferences 2024 Australia
Heart Diseases Conferences
Clinical Cardiology Conferences
Heart Congress Japan
Cardiac Imaging Conferences
Cardiology Conferences 2024
Cardiology Conferences 2024
Cardiology Conferences 2024 Asia
Hypertension Conferences
Pediatric Cardiology Conferences
Cardiology Conferences 2024
Dyslipidemia is a medical term used to describe an abnormal amount or distribution of lipids (fats) in the bloodstream. Cholesterol and triglycerides, which are carried in the blood as lipoproteins and are necessary parts of the body's cells, are examples of lipids. Usually, imbalance in these lipids' levels, particularly cholesterol, are referred to as dyslipidemia.
There are various kinds of lipoproteins, such as:
The lipid abnormalities that can be a part of dyslipidemia include:
Subtopics
LDL Cholesterol | HDL Cholesterol | NON-HDL Cholesterol | High Sensitivity C-Reactive Protein for Risk Assessment | Stratification of Dyslipidemia Risk | Advanced Lipoprotein Testing | Drugs for Treatment of Blood Lipoprotein Abnormalities
Market Statistics:
The global dyslipidemia drug market was worth US$ 11.8 billion in 2018 and is expected to grow at a CAGR of 3.5% from 2019 to 2027.
North America is the leading contributor to the dyslipidemia medications market. According to the Centers for Disease Control and Prevention (CDC), over 95 million adults in the United States (55% of the population) had total cholesterol levels greater than 200 mg/dL as of 2016. Furthermore, total cholesterol levels higher than 240 mg/dL affect an estimated 29 million adults in the United States.
Tags
Cardiac Imaging Conferences
Cardiology Conferences 2024 Asia
Heart Conferences
Heart Congress Japan
Cardiology Conferences USA
Peers Alley Media Conferences
Pediatric Cardiology Conferences
Hypertension Conferences
Cardiology Conferences 2024
Cardiology Conferences 2024 Canada
Cardiology Conferences 2024
Cardiology Conferences 2024 Australia
Stroke Conferences
Cardiac Surgery Conferences
Heart Diseases Conferences
Cardiovascular disease (CVD) refers to a class of diseases affect the heart or blood vessels, including the arteries and veins. Heart disease is another popular name for it. Among the biggest causes of death and disability in the globe are cardiovascular diseases.
The following are a few of the most prevalent heart conditions:
Subtopics:
Endocrine Functions and Metabolic Interactions | Endothelial dysfunction and clinical syndromes | Aging and Cognitive Function | Lipoproteins | Kidney and Hypertension | Atherosclerosis and colonary artery disease | Life style choices, Risk Factors | Diet and Homocysteinemia | Contribution of pollutants and Environmental Chemicals | Genetic Susceptibility | Precautions coronary interventions and Cardiac Surgery | Omega 3 fatty acid in prevention
Market Statistics:
The cardiovascular disease market, which includes hypertension, dyslipidemia, and thrombotic events, is expected to expand from $129.2 billion in 2015 to $146.4 billion by 2022.
The global cardiovascular devices market is expected to grow at a 6.9% CAGR from USD 54.08 billion in 2021 to USD 86.27 billion in 2028.
The global cardiovascular medicines market is predicted to increase at a CAGR of 5.3% from $87.79 billion in 2020 to $92.41 billion in 2021. The increase is primarily due to companies reorganising their operations and recovering from the impact of COVID-19. At a CAGR of 4%, the market is estimated to reach $107.77 billion in 2025.
Tags
Heart Diseases Conferences
Hypertension Conferences
Arrhythmia Conferences
Cardiology Conferences USA
Cardiology Conferences 2024
Heart Conferences
Cardiac Nursing Conferences
Stroke Conferences
Cardiac Surgery Conferences
Peers Alley Media Conferences
Cardiology Conferences 2024 Asia
Cardiac Imaging Conferences
Congestive heart failure (CHF), commonly referred to as heart failure, is a medical disorder when the heart is unable to effectively pump blood to satisfy the needs of the body. It happens when the heart's pumping power becomes weakened, causing an accumulation of fluid in the lungs and other body regions. Congestion and other symptoms may result from this fluid buildup.
The two primary varieties of congestive heart failure are as follows:
Congestive heart failure has a number of common causes and risk factors, including:
Congestive heart failure symptoms might differ, but frequently include:
Subtopics
Epidemiology & pathophysiology of heart failure | Differential Diagnosis of Congestive heart failure | Pharmacologic theraphy of Heart Failure | Clinical approach to acute heart failure | Clinical approach to chronic heart failure | The diagnosis and management of Congestive heart failure
Tags
Heart Conferences
Cardiac Imaging Conferences
Cardiology Conferences 2024 Canada
Cardiology Conferences USA
Hypertension Conferences
Vascular Biology Conferences
Heart Congress Japan
Cardiology Conferences 2024
Clinical Cardiology Conferences
Arrhythmia Conferences
Heart Diseases Conferences
Cardiology Conferences 2024
Cardiology Conferences 2024
Stroke Conferences
Acute Coronary Syndrome (ACS) is a term given to a variety of conditions when there is a sudden decrease in blood flow to the heart muscle because of a blockage of one or more coronary arteries. A variety of clinical manifestations, including unstable angina and myocardial infarction (heart attack), might result from this. ACS is a medical emergency that needs to be diagnosed and treated promptly.
Within the ACS spectrum, there are three primary conditions:
Typical symptoms of ACS include:
Subtopics
Reduction of Atherothrombosis for Continued Heath | Pathogenesis: Acute Coronary Syndrome | Molecular Mechanisms: Acute Coronary Syndrome | Immune System in Acute Coronary Syndrome | Myocardial Cell Death and Regeneration | Pharmacogenomics | Acute Ischemic Heart Disease | Echocardiography in Acute Coronary Syndrome | Nuclear Cardiology Techniques in Acute Coronary Syndrome | Plaque Passivation and Endothelial Therapy | The Modern Cardiac Unit | Antiplatelet Therapy | Anticoagulants
Tags
Cardiology Conferences 2024
Heart Congress Japan
Cardiac Surgery Conferences
Clinical Cardiology Conferences
Cardiology Conferences 2024
Hypertension Conferences
Cardiac Nursing Conferences
Cardiologist Conferences
Pediatric Cardiology Conferences
Cardiology Conferences 2024 Asia
Cardiac Imaging Conferences
Heart Conferences
Cardiology Conferences 2024
Cardiology Conferences 2024 Canada
Heart Diseases Conferences
Over the years, Innovations in cardiovascular surgery have greatly enhanced patient outcomes and lessened the invasiveness of treatments. These developments cover a range of surgical technology, surgical methods, and patient care.
Following are some notable advances in cardiovascular surgery:
Tags
Cardiology Conferences 2024
Cardiology Conferences 2024 Europe
Hypertension Conferences
Cardiology Conferences 2024 Australia
Vascular Biology Conferences
Pediatric Cardiology Conferences
Clinical Cardiology Conferences
Stroke Conferences
Heart Congress Japan
Cardiology Conferences 2024 Asia
Cardiology Conferences USA
Peers Alley Media Conferences
Cardiac Imaging Conferences
Heart-related disorders can be evaluated and diagnosed using cardiac biomarkers and diagnostic tools. These instruments aid medical personnel in the diagnosis of heart conditions, assessment of their severity, and direction of therapeutic options.
The following list of frequently used cardiac biomarkers and diagnostic devices:
1. Cardiac Biomarkers:
2. Electrocardiogram (ECG or EKG): An ECG records the electrical activity of the heart. It aids in the diagnosis of arrhythmias, conduction abnormalities, and heart attack warning symptoms. Depending on the clinical context, various ECGs, including 12-lead and Holter monitoring, are used.
3. Echocardiogram: An echocardiogram is an ultrasound test that produces images of the structure and function of the heart. It is used to evaluate the heart's ability to pump blood, evaluate the performance of its valves, and find abnormalities such cardiomyopathies.
4. Cardiac Catheterization: Cardiac catheterization entails inserting a thin, flexible tube (catheter) into a blood vessel and directing it to the heart. This treatment can be used to identify coronary artery disease, measure the heart's blood pressure, and carry out procedures including angioplasty and stent implantation.
5. Cardiac CT (Computerized Tomography) and MRI (Magnetic Resonance Imaging): These imaging methods techniques precise pictures of the heart and blood arteries. They are employed in the diagnosis of coronary artery disease, the evaluation of cardiac anatomy, and assessment of the severity of heart attack damage.
6. Stress Testing: Stress tests, such as pharmacological stress tests and exercise stress tests, measure how the heart reacts to physical strain or medication. They are used to determine exercise tolerance and detect coronary artery disease.
7. Coronary Angiography: Coronary angiography is a process in which contrast dye is injected into the coronary arteries, and X-ray images are then taken. It is used to visualize coronary artery blockages or narrowing.
8. Blood Lipid Profile: This consists of measurements of cholesterol levels, high-density lipoprotein (HDL) and low-density lipoprotein (LDL) cholesterol, as well as triglycerides. Atherosclerosis and coronary artery disease are both risk factors for abnormal lipid levels.
9. Chest X-ray: A chest X-ray can show the shape and size of the heart as well as identify diseases like congestive heart failure or lung issues that may be damaging the heart.
10. Genetic Testing: Genetic tests may be used to discover inherited cardiac diseases that can raise the risk of heart problems, such as hypertrophic cardiomyopathy or long QT syndrome.
Tags
Cardiology Conferences USA
Clinical Cardiology Conferences
Heart Conferences
Stroke Conferences
Cardiac Surgery Conferences
Cardiology Conferences 2024 Australia
Cardiac Nursing Conferences
Cardiology Conferences 2024
Cardiology Conferences 2024
Cardiologist Conferences
Pediatric Cardiology Conferences
Cardiology Conferences 2024 Europe
Cardiac Imaging Conferences
Hypertension Conferences
Cardiogenomics is a branch of study that focuses on how genetics and cardiology interact, particularly how a person's genetic makeup influences their risk of developing cardiovascular illnesses (CVDs) and how well they respond to treatment. It is essential in the creation of individualized treatment plans for cardiovascular diseases.
The contribution of cardiogenomics to individualized care is summarized as follows:
Tags
Cardiology Conferences 2024 Asia
Heart Congress Japan
Cardiac Surgery Conferences
Cardiology Conferences 2024
Cardiology Conferences 2024 Canada
Cardiology Conferences 2024
Cardiac Nursing Conferences
Vascular Biology Conferences
Heart Diseases Conferences
Arrhythmia Conferences
Hypertension Conferences
Heart Conferences
Cardiovascular epidemiology is a subfield of epidemiology that focuses on the investigation of cardiovascular diseases (CVDs) in populations. It aims to understand the prevalence of cardiac diseases and other ailments in the population as well as their causes, risk factors, and prevention. On the other hand, public health focuses on efforts to improve the overall well-being and health of communities and populations.
Several important aspects of cardiovascular epidemiology and its relationship to public health are listed below:
Tags
Cardiology Conferences 2024 Canada
Cardiologist Conferences
Hypertension Conferences
Cardiology Conferences 2024
Arrhythmia Conferences
Heart Conferences
Cardiology Conferences 2024 Europe
Cardiology Conferences USA
Peers Alley Media Conferences
Clinical Cardiology Conferences
Heart Congress Japan
Cardiology Conferences 2024
Heart Diseases Conferences
Cardiology Conferences 2024 Asia
Cardiac Surgery Conferences
A variety of heart-related conditions can be diagnosed, treated, and managed with the use of cardiac devices and implanted technologies. These devices are made to keep track of the heart's activities, regulate its rhythm, and facilitate its function.
The following are some essential cardiac devices and implanted technologies:
Tags
Cardiac Surgery Conferences
Cardiology Conferences 2024
Heart Conferences
Cardiology Conferences USA
Cardiology Conferences 2024 Canada
Heart Diseases Conferences
Cardiology Conferences 2024 Australia
Peers Alley Media Conferences
Cardiac Imaging Conferences
Cardiology Conferences 2024
Hypertension Conferences
Cardiologist Conferences
Maintaining heart health and lowering the risk of heart diseases, such as heart attacks and strokes, depend heavily on cardiovascular risk assessment and prevention. These methods seek to recognize at-risk individuals and put into place measures to lessen their risk factors. Detailed information about determining cardiovascular risk and preventing it is provided below:
1. Risk Factors for Cardiovascular Disease:
Modifiable risk factors include: Through dietary adjustments and medical treatment, these can be controlled or modified.
Non-modifiable risk factors include: These can't be changed, but they should be taken into account when evaluating overall risk.
2. Cardiovascular Risk Assessment:
3. Prevention Strategies:
Lifestyle Modifications:
Medications: Medicines may be administered to treat illnesses including hypertension, high cholesterol, or diabetes in people with particular risk factors or a history of cardiovascular events.
Aspirin Therapy: Some people may be advised to take aspirin, but before doing so, users should carefully assess their own risk factors and potential bleeding concerns.
Surgery or Intervention: In severe cases, procedures like percutaneous coronary intervention (PCI) or coronary artery bypass grafting (CABG) may be necessary to open blocked arteries.
Cardiac Rehabilitation: Programs that include physical activity, education, and counseling to aid people in recovering from heart illness or surgery and enhancing their heart health.
Regular Check-Ups: For early detection and intervention, regular medical checkups and monitoring of risk factors are essential.
4. Patient Education and Counseling:
5. Community-Based Programs:
Through education, access to healthy diets, and opportunities for physical activity, community programs and public health initiatives can encourage heart-healthy lives.
6. Monitoring and Adherence:
Tags
Cardiology Conferences 2024 Europe
Vascular Biology Conferences
Cardiology Conferences 2024 Canada
Cardiac Nursing Conferences
Peers Alley Media Conferences
Pediatric Cardiology Conferences
Cardiac Surgery Conferences
Heart Diseases Conferences
Cardiologist Conferences
Heart Congress Japan
Cardiology Conferences 2024
Stroke Conferences
Clinical Cardiology Conferences
Cardiology Conferences 2024
Hypertension Conferences

Big data and analytics are playing a bigger role in cardiology and have completely changed how health care professionals diagnose, treat, and manage cardiovascular diseases.
The following are some significant applications of big data and analytics in cardiology:
1. Predictive Analytics for Risk Assessment:
2. Personalized Medicine:
3. Remote Monitoring and Wearables:
4. Image Analysis:
5. Drug Discovery and Development:
6. Population Health Management:
7. Quality Improvement and Benchmarking:
8. Research and Clinical Trials:
9. Data Security and Privacy:
Tags
Cardiology Conferences 2024
Peers Alley Media Conferences
Cardiac Surgery Conferences
Pediatric Cardiology Conferences
Cardiac Nursing Conferences
Heart Congress Japan
Stroke Conferences
Vascular Biology Conferences
Cardiology Conferences 2024 Australia
Heart Conferences
Cardiology Conferences 2024
Clinical Cardiology Conferences
Arrhythmia Conferences
Cardiology Conferences 2024 Asia
Artificial heart devices and heart transplants are two key treatments for end-stage heart failure, a condition in which the heart is no longer able to properly pump blood. Both treatments have advantages and disadvantages, and the therapy chosen is based on the patient's individual medical condition and needs.
1. Artificial Heart Devices (Ventricular Assist Devices - VADs):
2. Heart Transplants:
Tags
Cardiologist Conferences
Cardiac Imaging Conferences
Cardiac Nursing Conferences
Cardiology Conferences 2024
Cardiology Conferences 2024 Canada
Arrhythmia Conferences
Cardiology Conferences USA
Heart Congress Japan
Cardiology Conferences 2024 Australia
Clinical Cardiology Conferences
Heart Conferences
Cardiology Conferences 2024
Cardiology Conferences 2024 Europe
Pediatric Cardiology Conferences
Cardiac imaging plays a crucial role in risk prediction and the management of cardiovascular diseases (CVDs). It enables healthcare professionals to evaluate the heart's structure and functioning, spot abnormalities, and predict the likelihood of future cardiovascular problems.
The following are some popular cardiac imaging techniques for risk assessment:
1. Echocardiography (Echo):
2. Stress Testing:
3. Cardiac CT Angiography (CTA): Computed tomography (CT) technology is used during CTA to produce DETAILED pictures of the coronary arteries. It can identify coronary artery calcifications, which are linked to higher risk, as well as the presence of coronary artery disease and the severity of stenosis (narrowing).
4. Cardiac MRI (CMR): CMR provides high-resolution images of the heart's structure and function. It can measure the size of the heart chambers, assess myocardial viability, and evaluate cardiac performance. For a variety of cardiac conditions, CMR can be useful in predicting risk.
5. Coronary Calcium Scoring (CAC): The amount of calcium deposits in the coronary arteries are measured using this specific CT scan. A high CAC score suggests an increased risk of future cardiovascular events and coronary artery disease.
6. Cardiac PET Scan: Positron emission tomography (PET) scans can offer details on the metabolism and blood flow in the heart. It is frequently used to assess the viability and perfusion of the myocardium.
7. Cardiac Catheterization (Angiography): Despite being invasive, cardiac catheterization is still a gold standard for detecting coronary artery disease. It gives precise images of the coronary arteries and can guide interventions like angioplasty or stent placement.
8. Cardiac Biomarkers: Blood testing for cardiac biomarkers like troponin and B-type natriuretic peptide (BNP) are crucial for risk assessment in addition to imaging. These biomarkers' elevated levels may indicate cardiac stress or damage.
Tags
Cardiac Surgery Conferences
Heart Diseases Conferences
Peers Alley Media Conferences
Vascular Biology Conferences
Cardiology Conferences 2024 Canada
Cardiology Conferences 2024
Hypertension Conferences
Stroke Conferences
Heart Congress Japan
Cardiologist Conferences
Cardiology Conferences 2024
Cardiology Conferences USA
Arrhythmia Conferences
In order to give a more comprehensive and patient-centered approach to heart health, integrative medicine in cardiology is an approach to cardiovascular care that combines conventional medical treatments with complementary and alternative therapies. It recognises the significance of addressing not only the physical components of heart disease but also the emotional, psychological, and lifestyle issues that can affect cardiovascular health.
The following are some important aspects of integrative medicine in cardiology:
Tags
Peers Alley Media Conferences
Pediatric Cardiology Conferences
Cardiac Imaging Conferences
Cardiology Conferences 2024 Europe
Vascular Biology Conferences
Clinical Cardiology Conferences
Hypertension Conferences
Stroke Conferences
Cardiac Nursing Conferences
Cardiology Conferences USA
Cardiac Surgery Conferences
Heart Diseases Conferences
Cardiology Conferences 2024
Cardiology Conferences 2024 Asia
The field of cardiology is one that is undergoing tremendous change at the moment. People living in this era, regardless of age, are at risk for developing cardiovascular diseases, the primary causes of which are the lifestyles they lead and the lack of proper hygiene they practise. Cardiology has become more important over time as a way to fight these diseases and the things that cause them. Interventional cardiology is a subspecialty of cardiology that treats disorders through the use of catheter-based minimally invasive treatments. This enables both patients and their treating physicians to complete the surgery with less blood loss and minor complications.
Some scientific advances in the fields of sciences, interventional cardiology, and cryopreservation are also predicted to drive the cardiac surgery devices market. The use of expanded Polytetrafluoroethylene for cardiovascular patches, the introduction of transcatheter heart valves, and thus the process of minimally invasive technologies, such as transcatheter semi-lunar valve implantation or transcatheter aortic valve replacement, are just a few of the factors that are expected to drive growth over the forecast period. Furthermore, changes in cryopreservation technologies by key players like CryoLife are among major technological breakthroughs in cardiac surgery therapies that are expected to positively influence the market.
The presence of technologically advanced cardiology and cardiovascular valves, grafts, and patches, as well as an increase in the generality of congenital heart defects, are among the basic variables projected to drive development over the forecast period. During the projection period of 2017-2023, the global market for heart transplants is expected to develop at a CAGR (Compound Annual Growth Rate) of 11.2 percent. The global Interventional Cardiology market is expected to develop slowly at a CAGR of almost 7% during the forecast period. The increased need for minimally invasive (MI) procedures will boost the global interventional cardiology market's growth prospects in the future years.The global interventional cardiology devices market is expected to be worth USD 21.2 billion by 2025, up from USD 13.8 billion in 2020, at an 8.9 percent CAGR during the forecast period. The significant rise in the geriatric population, prevalence of coronary artery diseases, the approval of new and sophisticated products, and thus the rising incidence of diabetes, are all driving growth in this industry.
Cardiology Market in Asia-Pacific:
It is anticipated that the Asia Pacific Interventional Cardiology Market will reach USD 41,00.3 Million by the end of the estimated period (2020-2027), expanding at a compound annual growth rate (CAGR) of 8%.
According to the International Diabetes Federation, Asia is home to 60% of the world's diabetes population. Diabetes is one of the leading causes of cardiovascular disease. The rising prevalence of cardiovascular illnesses is the primary driver of market growth in Asia Pacific. Aside from the rising prevalence of diabetes and obesity, changes in lifestyle, more public awareness, and quick technological advancements all contributed to the market's expansion. On the other hand, high cost for manufacturing the devices and a lot of barriers for the course of the new device are the main restraints hampering the market growth.
Abbott Laboratories, Becton, Dickinson and Company, Boston Scientific Corporation, Edwards Lifesciences Corporation, Medtronic PLC, and Terumo Corporation are some of the firms that are aiding in the expansion of the market for cardiovascular devices in the Asia-Pacific region.
Cardiology Market in Europe:
The Europe region market for Cardiology management devices, Aortic Repair devices, transcatheter embolization and occlusion devices will grow through 2026, driven by factors such as an ageing population, sedentary lifestyle and changes in food habits, advancements in the field of cardiology as well as an increase in the number of interventional cardiologists, and increasing demand for surgical occlusion devices.
The European Interventional Cardiology Market shrank by roughly 27% from 2019 as a result of COVID19, with a valuation of about €928 million in 2020. In 2022, the market size is anticipated to surpass pre-COVID19 levels, and in 2026, it will reach €1 billion.
In the year 2022, the total market size for cardiovascular devices in the European region was estimated to be worth USD 14.47 billion. It is further anticipated that this value would increase at a compound annual growth rate of 6.42 percent from 2022 to 2027, reaching a value of USD 19.75 billion by 2027.In the year 2022, the total market size for cardiovascular devices in the European region was estimated to be worth USD 14.47 billion. It is further anticipated that this value would increase at a CAGR of 6.42% from 2022 to 2027, reaching a value of USD 19.75 billion by 2027.
Geographically, North America has the highest market share in 2019 due to increased awareness of gut illnesses. According to the Centers for Disease Control and Prevention (CDC), approximately 610,000 Americans die of heart disease each year. Similarly, 735,000 Americans die of heart attacks each year. Thus, an increase in heart attacks in North America would increase the demand for cardiovascular drugs. However, Asia-Pacific region is predicted to showcase the fastest rate of growth within the future due to the rise in the aging population, increasing awareness and other factors.
The global market for cardiovascular devices is projected to increase from $48.10 billion in 2021 to $76.52 billion in 2028, representing a CAGR of 6.9% for the forecast period of 2021-2028.
Cardiology Market in Middle East:
Countries in the Middle East and Africa bear an important burden from Ischemic heart conditions. Consistent with Dubai Health Authority, heart condition is the cause for each 3 in 10 deaths within the UAE. Huge funding in R&D and various initiatives by the government is driving the expansion of the Ischemic heart condition market in the Middle East and Africa. The Middle-East and Africa Ischemic heart condition market is growing steadily. The market is growing at the CAGR of three .1% and expected to succeed in to US$ 2.84 billion by 2022.
In the forecasted period of 2022 to 2029, the Middle East interventional cardiology and peripheral vascular devices market is anticipated to develop. According to Data Bridge Market Research's analysis, the market is expanding with a CAGR of 5.3% from 2022 to 2029 and is anticipated to rise from USD 400.11 million in 2021 to USD 579.59 million by that time. Increased prevalence of ischemic heart disease, vascular disease, and coronary artery disease, as well as a rise in public awareness of the need for prompt diagnosis and usage of devices, are projected to be the main factors driving market demand throughout the forecast period.
In 2018, the market for cardiovascular devices in China was worth USD 2,837.51 million. By 2024, it is expected to be worth USD 4,468.02 million, with a CAGR of 7.86 percent over the next five years.
Future Cardiology reflects this new era of cardiology and highlights the new molecular approach to advancing cardiovascular therapy. Coverage also will reflect the main technological advances in bioengineering in cardiology in terms of advanced and robust devices, miniaturization, imaging, system modeling and knowledge management issues.
Cardiology Journals | Cardiology Open Access
Journal of the American College of Cardiology / JAMA Cardiology / Circulation / Nature Reviews Cardiology / JACC: Cardiovascular Imaging / JACC: Heart Failure / European Journal of Heart Failure / Circulation Research / European Heart Journal / JACC: Cardiovascular Interventions / Circulation: Heart Failure / Stroke / Circulation: Cardiovascular Interventions / JACC: Basic to Translational Science / European Heart Journal Cardiovascular Imaging / Cardiovascular Research / Arteriosclerosis, Thrombosis, and Vascular Biology / American Heart Journal / Circulation: Cardiovascular Quality and Outcomes / Journal of Heart and Lung Transplantation / Circulation: Arrhythmia and Electrophysiology / Cardiovascular Diabetology / Circulation. Genomic and precision medicine / Heart Rhythm / Journal of the American Society of Echocardiography / Chest / Journal of the American Heart Association / Journal of Cardiovascular Magnetic Resonance / Resuscitation / Circulation: Cardiovascular Imaging / Heart / JACC: Clinical Electrophysiology / Journal of Stroke / European Stroke Journal / Progress in Cardiovascular Diseases / Journal of Cerebral Blood Flow and Metabolism / Current Problems in Cardiology / Europace / Stroke and Vascular Neurology / Journal of Vascular Surgery / GeroScience / Trends in Cardiovascular Medicine / Clinical Research in Cardiology / European heart journal. Quality of care & clinical outcomes / European Journal of Preventive Cardiology / JACC: CardioOncology / EuroIntervention / European Heart Journal - Cardiovascular Pharmacotherapy / Basic Research in Cardiology / American Journal of Physiology - Heart and Circulatory Physiology / European Heart Journal: Acute Cardiovascular Care / Journal of Molecular and Cellular Cardiology / Interventional Neurology / Frontiers in Cardiovascular Medicine / Translational Stroke Research / Journal of Cardiac Failure / Atherosclerosis / Journal of Thoracic and Cardiovascular Surgery / Canadian Journal of Cardiology / European Journal of Vascular and Endovascular Surgery / Current Atherosclerosis Reports / Journal of Clinical Lipidology / Journal of Atherosclerosis and Thrombosis / Journal of Cardiovascular Computed Tomography / Journal of Endovascular Therapy / International Journal of Cardiology / Seminars in Thrombosis and Hemostasis / European Journal of Cardio-thoracic Surgery / Heart Failure Reviews / Hypertension Research / American Journal of Cardiology / Journal of Hypertension / Current Opinion in Lipidology / Annals of Thoracic Surgery / Catheterization and Cardiovascular Interventions / Interventional Cardiology Review / Arrhythmia and Electrophysiology Review / Vascular Medicine / Journal of Cardiovascular Electrophysiology / Nutrition, Metabolism and Cardiovascular Diseases / American Journal of Cardiovascular Drugs / Clinical Cardiology / Journal of Thrombosis and Thrombolysis / European Cardiology Review / Circulation Journal / Current Cardiology Reports / Journal of Vascular and Interventional Radiology / Open Heart / Vascular Health and Risk Management / Journal of Clinical Hypertension / Cardiovascular Intervention and Therapeutics / Cardiovascular Drugs and Therapy / Journal of Cardiology / Journal of Cardiopulmonary Rehabilitation and Prevention / Journal of Nuclear Cardiology / Cerebrovascular Diseases / Archives of Cardiovascular Diseases / Therapeutic Advances in Cardiovascular Disease / CPT: Pharmacometrics and Systems Pharmacology / Korean Circulation Journal / European Journal of Cardiovascular Nursing / Cardiovascular Pathology / Clinical Medicine Insights: Cardiology / IJC Heart and Vasculature / Global Heart / ESC heart failure / Cardiology and Therapy / Diabetes and Vascular Disease Research / Journal of Vascular Surgery: Venous and Lymphatic Disorders / Journal of Cardiovascular Translational Research / Netherlands Heart Journal / High Blood Pressure and Cardiovascular Prevention / Neuroradiology / Heart Lung and Circulation / Cardiovascular Therapeutics / Current Treatment Options in Cardiovascular Medicine / Diagnostic and Interventional Radiology / Cerebrovascular Diseases Extra / CardioVascular and Interventional Radiology / Kidney and Blood Pressure Research / Journal of Geriatric Cardiology / Cardiovascular Endocrinology and Metabolism / Journal of Stroke and Cerebrovascular Diseases / International Journal of Cardiovascular Imaging / Journal of Cardiovascular Pharmacology / JMIR Cardio / Journal of Cardiovascular Pharmacology and Therapeutics / Journal of Interventional Cardiology / Microvascular Research / Cardiology Research / Journal of Interventional Cardiac Electrophysiology / BMC Cardiovascular Disorders / Congenital Heart Disease / Current Vascular Pharmacology / Microcirculation / Lymphatic Research and Biology / Expert Review of Cardiovascular Therapy / Seminars in Thoracic and Cardiovascular Surgery / Cardiovascular Diagnosis and Therapy / Cardiac Failure Review / Cardiovascular Ultrasound / Heart Failure Clinics / Current Opinion in Cardiology / Journal of the American Society of Hypertension / Angiology / Heart and Lung: Journal of Acute and Critical Care / Hellenic Journal of Cardiology / Integrated Blood Pressure Control / Interventional Neuroradiology / Current Heart Failure Reports / Cardiology in Review / Evidence and Policy / Clinical Medicine Insights: Circulatory, Respiratory and Pulmonary Medicine / Pediatric Cardiology / CardioRenal Medicine / Interventional Cardiology Clinics / CJC Open / Reviews in Cardiovascular Medicine / PACE - Pacing and Clinical Electrophysiology / Journal of Cardiothoracic and Vascular Anesthesia / Journal of Cardiovascular Surgery / Journal of Invasive Cardiology / Cardiology Journal / Heart Asia / Journal of Cardiovascular Imaging / Cardiovascular Toxicology / Journal of Cardiovascular Nursing / Current Cardiology Reviews / Heart and Vessels / Cardiology Clinics / Annals of Cardiothoracic Surgery / Pediatric Cardiac Surgery Annual / Cardiovascular Engineering and Technology / International Angiology / Cardiology / Interactive Cardiovascular and Thoracic Surgery / REC: Interventional Cardiology / Clinical Hemorheology and Microcirculation / Annals of Vascular Surgery / Journal of Lipid and Atherosclerosis / Phlebology / Innovations: Technology and Techniques in Cardiothoracic and Vascular Surgery / Journal of Arrhythmia / Annals of Thoracic Medicine / Cardiovascular Revascularization Medicine / Techniques in Vascular and Interventional Radiology / Journal of Innovations in Cardiac Rhythm Management / Acta Myologica / Vasa - European Journal of Vascular Medicine / Annals of Thoracic and Cardiovascular Surgery / Perfusion (United Kingdom) / European Heart Journal, Supplement / Kardiologia Polska / Cardiology Research and Practice / International Heart Journal / Echocardiography / Indian Heart Journal / Vascular and Endovascular Surgery / Thoracic and Cardiovascular Surgeon / Cardiac Electrophysiology Clinics / Journal of Vascular Research / Seminars in Interventional Radiology / Journal of Electrocardiology / Cardiovascular and Hematological Agents in Medicinal Chemistry / Revista Espanola de Cardiologia / General Thoracic and Cardiovascular Surgery / Journal of Cardiovascular Medicine / Monaldi Archives for Chest Disease / Scandinavian Cardiovascular Journal / International Journal of Cardiology: Hypertension / Blood Pressure / Seminars in Vascular Surgery / Coronary Artery Disease / Acta Cardiologica Sinica / Acta Cardiologica / Journal of Cardiac Surgery / Vascular / Critical Pathways in Cardiology / Annals of Noninvasive / Electrocardiology / Atherosclerosis Plus / Herz / Anatolian journal of cardiology / Indian Pacing and Electrophysiology Journal / Blood Pressure Monitoring / Minerva Cardiology and Angiology / World Journal of Cardiology / Journal of Cardiothoracic Surgery / World journal for pediatric & congenital heart surgery / Future Cardiology / Journal of Atrial Fibrillation / HeartRhythm Case Reports / Journal of Artificial Organs / Arquivos Brasileiros de Cardiologia / Clinica e Investigacion en Arteriosclerosis / Cardiology in the Young / International Journal of Vascular Medicine / International Journal of Angiology / Journal of Extra-Corporeal Technology / Operative Techniques in Thoracic and Cardiovascular Surgery / Texas Heart Institute Journal / Brazilian Journal of Cardiovascular Surgery / Egyptian Heart Journal / Cardiovascular and Hematological Disorders - Drug Targets / Cardiovascular Journal of Africa / Annals of Pediatric Cardiology / Seminars in Cardiothoracic and Vascular Anesthesia / Vascular Specialist International / Archives of Clinical Infectious Diseases / JMV-Journal de Medecine Vasculaire / Postepy w Kardiologii Interwencyjnej / Annals of Cardiac Anaesthesia / European Heart Journal - Case Reports / Journal of Heart Valve Disease / Journal of Vascular Surgery Cases and Innovative Techniques / ARYA Atherosclerosis / Open Cardiovascular Medicine Journal / Computing in Cardiology / EJVES Vascular Forum / Artery Research / Revista Portuguesa de Cardiologia / Jornal Vascular Brasileiro / Journal of Cardiology Cases / Phlebologie / Complex Issues of Cardiovascular Diseases / Chinese Journal of Cardiology / Journal of Cardiovascular and Thoracic Research / Journal of Cardiovascular Echography / Turk Kardiyoloji Dernegi Arsivi / Heart Surgery Forum / Structural Heart / CVIR Endovascular / JACC: Case Reports / Turkish Journal of Thoracic and Cardiovascular Surgery / Journal of the Saudi Heart Association / Asian Cardiovascular and Thoracic Annals / Kardiochirurgia i Torakochirurgia Polska / Korean Journal of Thoracic and Cardiovascular Surgery / Heart International / Flebologiya / Electrolyte and Blood Pressure / Cardiovascular Therapy and Prevention (Russian Federation) / Giornale Italiano di Cardiologia / Kardiologe / US Cardiology Review / Vascular Disease Management / Kardiologiya / Annales de Cardiologie et d'Angeiologie / Russian Journal of Cardiology / Gefasschirurgie / Herzschrittmachertherapie und Elektrophysiologie / Progress in Pediatric Cardiology / Arterial Hypertension / Journal of Tehran University Heart Center / Thoracic and Cardiovascular Surgeon, Supplement / Hipertension y Riesgo Vascular / Rational Pharmacotherapy in Cardiology / Cor et Vasa / Patologiya Krovoobrashcheniya i Kardiokhirurgiya / International Cardiovascular Research Journal / Acta Phlebologica / Arterial Hypertension (Russian Federation) / Cirugia Cardiovascular / Kardiologiya i Serdechno-Sosudistaya Khirurgiya / Indian Journal of Thoracic and Cardiovascular Surgery / Cardiology Letters / Italian Journal of Vascular and Endovascular Surgery / AORTA / Vnitrni Lekarstvi / REC: CardioClinics / Revista Argentina de Cardiologia / Atherosclerosis: X / Archivos de Cardiologia de Mexico / Angiologia / Iranian Heart Journal / Revista Espanola de Cardiologia Suplementos / Insuficiencia Cardiaca / Revista Mexicana de Angiologia / Acta Angiologica / Revista de la Federacion Argentina de Cardiologia / Revista Colombiana de Cardiologia / Revista Latinoamericana de Hipertension / Journal for Vascular Ultrasound / Medecine des Maladies Metaboliques / British Journal of Cardiology / Clinical Lipidology and Metabolic Disorders / Revista Mexicana de Cardiologia / Pakistan Heart Journal / Shanghai Chest / Zeitschrift fur Herz-, Thorax- und Gefasschirurgie / Open Hypertension Journal / Vasomed / Kardiologija v Belarusi / Zeitschrift fur Gefassmedizin / Chinese Journal of Cerebrovascular Diseases / Journal of the Hong Kong College of Cardiology / Heart and Metabolism / Intervencni a Akutni Kardiologie / Archives of Cardiovascular Diseases Supplements / European Journal of Lymphology and Related Problems / Lymphologie in Forschung und Praxis / Revista Cubana de Cardiologia y Cirugia Cardiovascular / Turkiye Klinikleri Cardiovascular Sciences / Dialogues in Cardiovascular Medicine / Kardiotechnik / Perfusion (Germany) / Archives des Maladies du Coeur et des Vaisseaux – Pratique / Journal of Rare Cardiovascular Diseases / Kardiologicka Revue / Cardiovascular Medicine(Switzerland) / Clinical Hypertension
Heart Disease Organizations Worldwide | Cardiology Associtations
Abiomed / Alliance for Heart Failure / American Academy of Cardiovascular Perfusion / American College of Cardiology / American Heart Association / American Society of Nuclear Cardiology / Association for Inherited Cardiac Conditions / Atrial Fibrillation Association / Baker Heart and Diabetes Institute / Blood Pressure Association / British Cardiovascular Society / British Heart Foundation / Canadian Cardiovascular Society / Cardiac Risk in the Young / Cardiovascular Cell Therapy Research Network / Cardiovascular System Dynamics Society / Children's Cardiomyopathy Foundation / Congenital Heart Surgeons' Society / Corindus Vascular Robotics / Deutsche Gesellschaft für Kardiologie / European Association for Cardio-Thoracic Surgery / European Society of Cardiology / GISSI / Heart and Diabetes Center North Rhine-Westphalia / Heart and Stroke Foundation of Canada / Heart Failure Society of America / Heart Institute, University of São Paulo / Heart Research Institute / Heart Research UK / Heart Rhythm Society / Heart Support of America / Indian Heart Association / Institute of Cardiovascular & Medical Sciences / Interamerican Society of Cardiology / International Society for Heart Research / Krishna Heart Institute / Libin Cardiovascular Institute of Alberta / Lourdes Heart Institute / Mended Hearts / Montreal Heart Institute / Montreal Heart Institute Foundation / Mount Sinai Medical Center (Miami) / Multan Institute of Cardiology / National Heart Forum / National Heart Foundation (Bangladesh) / National Heart Foundation of Australia / National Heart Foundation of New Zealand / National Heart Institute (Malaysia) / Philippine Heart Center / Pulmonary Hypertension Association / Punjab Institute of Cardiology / Rabindranath Tagore International Institute of Cardiac Sciences / Resuscitation Council UK / Society for Cardiovascular Magnetic Resonance / Sri Jayadeva Institute of Cardiovascular Sciences and Research / Surgeons of Hope / Tanzania Heart Institute / The Texas Heart Institute / Tiny Tickers / Uganda Heart Institute / United OneHeart Foundation / University of Ottawa Heart Institute / Victor Chang Cardiac Research Institute / West of Scotland Heart and Lung Centre
Contact us now and we will make your event unique & unforgettable
All numbers indicates percentage %
Europe
North America
Middle East
Asia Pacific
Africa
All numbers indicates percentage %
Cardiologists
Cardiovascular Surgeons
Healthcare Professionals
Nurse Practitioners
Scholars
Medical Students
BusinessIndustry
Manufacturing CompaniesHospitals

Aims: Cancer-induced cachexia affects up to 80% of patients with cancer. Patients with cancer-induced cachexia may experience cardiac wasting through inter-tissue and inter-organ crosstalk. This review aims to identify evidence of cancer-induced cardiac cachexia in human and non-human models by examining the contribution of biom
The incidence of sports-related sudden cardiac death is fourfold higher in persons over age 65 compared to the frequency of such events in the general population, as reported by Holmstrom, et al.1,2. Low-dose aspirin use may be appropriate to provide enhanced primary prevention of such fatalities as has been recommended to atten
Elevated sympathetic activity and chronic inflammation contribute to hypertension in both animals and patients. In previous studies, we have observed that sympathoinhibitory electroacupuncture (SI-EA) at acupoints S36-37 alleviates sympathetic activity and hypertension. Additionally, EA at acupoints SP6-7 exerts anti-inflammat

Severity of illness scores—Acute Physiology and Chronic Health Evaluation, Simplified Acute Physiology Score, and Sequential Organ Failure Assessment—are current risk stratification and mortality prediction tools used in intensive care units (ICUs) worldwide. Developers of artificial intelligence or machine learning (ML) mod

Background: The approach to hyponatremia is in a state of flux. Cerebral/renal salt wasting (RSW) is considered rare and presents with identical parameters as SIADH that create a diagnostic and therapeutic dilemma, whether to fluid-restrict water-logged patients with SIADH or administer saline to dehydrated patients with RSW. W
Dementia is experienced as the failing of the brain in an otherwise healthy body; its cause is still debated. In this talk I bring together evidence that several dementias (pugilistica, chronic traumatic encephalopathy, traumatic brain injury, Alzheimer's) share the common feature of widespread capillary haemorrhage, senile plaq
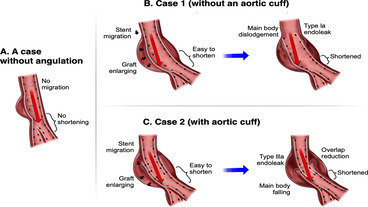
The Endologix® AFX® (Endologix, Inc., Irvine, CA, USA) endovascular abdominal aortic aneurysm (AAA) graft systems have a unique unibody structure suitable for narrow aortic bifurcations in AAAs.1 However, since 2017, the Food and Drug Administration has issued several safety warnings against its routine use for AAA treatment d
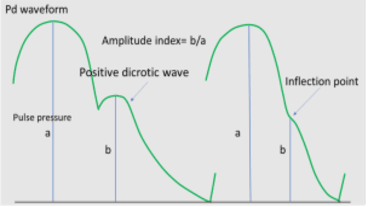
Background and aim: As coronary stenosis progresses, arterioles in the related myocardial region dilate in proportion to ischaemia, resulting in a decrease in resting distal coronary pressure/aortic pressure (Pd/Pa). However, we find some high-remaining resting Pd/Pa values with a large diremption from fractional flow rese
Backgrounds: Heart failure (HF) is a progressive syndrome characterized by complicated therapeutic regimens and repeated hospitalizations. HF has turned into a global epidemic demonstrating serious mortality and morbidity. This study aimed to assess the relationship between disease knowledge and selfcare adherence among adult HF